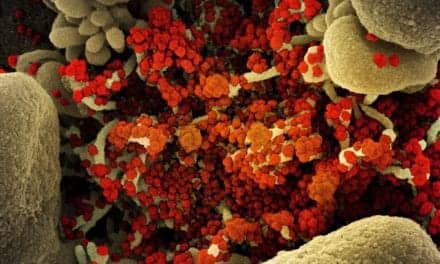
The COVID-19 pandemic has made business as usual a distant memory for many RTs, including the administration of respiratory support therapies like ventilation.
By Greg Thompson
More than two years after the start of the COVID pandemic, patients are still catching the virus but consequences are less severe. In the Pacific Northwest region of Tacoma, Wash, Karen LaRoche, RRT, ACCS has seen the progression firsthand.
“At this point, we are not seeing the critically ill patients in the numbers that we have in the past,” said LaRoche, respiratory clinical specialist at Multicare Health System. “The number of people admitted to the hospital who have COVID is pretty high, but the number of patients requiring mechanical ventilation, Bi-PAP therapy, and hi-flow nasal cannula therapy is very low. It’s mild illness.”
Home Monitoring of Patients
For the minority of patients who need care in the home, there has been a significant increase in telemonitoring and telehealth adoption since the pandemic began. In response, San Diego-based ResMed accelerated the launch of AirView for Ventilation, which enables remote monitoring of respiratory care patients on ResMed ventilators and bilevel devices.
“Clinicians can review data, refine device settings, and troubleshoot any issues post-initial setup,” explained Luciana Rabello de Oliveira, clinical director at ResMed. “Digital solutions like AirView for Ventilation help provide the best support solutions to clinicians and, in turn, the best care and experience for patients and their families.”
A 2021 review of AirView for Ventilation and similar solutions in the Annals of the American Thoracic Society concluded: “Quantitative home monitoring holds promise for improving precision in home ventilator management with the long-term goals of minimizing adverse events and maximizing patient quality of life. Widespread application of new noninvasive assessment tools could obviate emergency hospitalization for unrecognized chronic hypoventilation and might reduce admissions for acute or chronic hypercapnic respiratory failure.”
The challenges of ventilating COVID-19 patients stem from what Dan Dunmire, RRT, lead clinical specialist at Movair, Austin, Tex, explained is lung scarring and physiological changes. Specifically, the lungs are typically less compliant and “exhibit a restrictive disease process characterized by difficulty delivering appropriate volumes and decreased tissue elastance.” He added that the diffusion capacity of many patients is also diminished, impairing gas exchange and leading to hypoxemia and hypercapnia.
“Noninvasive ventilation has been used extensively for treatment of chronic respiratory conditions in the home and has found a place for treating COVID-19 as well,” Dunmire said. “Because the lungs are the organ most effected by COVID-19, noninvasive ventilation is used to promote more consistent tidal volume delivery, increase mean airway pressure, and aid gas exchange across the alveolar-capillary membrane. Patients experience a decreased work of breathing [WOB] as the ventilator helps to supplement volume delivery.”
These days, many patients at Washington-based Multicare are admitted for something else, tested for COVID, and find they are positive. With severity significantly less than what it was last Summer, LaRoche admits that everyone is breathing a sigh of relief. “The flip side is that the current COVID strain is easily spread and going through the community in droves,” she said. “We have staff becoming ill, and that means short-staffing scenarios. Those are some of the challenges that we still have related to COVID.”
Post-COVID Respiratory Support
LaRoche reiterates that very few patients have required post COVID mechanical ventilation at home. “Patients either did well when removed from the vent or they ultimately did not survive,” she confirms. “Bottom line is that we have not seen a lot of challenges specifically related to mechanical ventilation at home after having COVID. However, we have seen a marked increase in younger, healthier patients requiring oxygen at home.”
Many of these “younger” patients in their 40s and 50s require high-flow nasal cannula therapy, primarily due to residual shortness of breath paired with hypoxemia. According to LaRoche, these patients can walk effectively as long as they have oxygen, but without it they markedly desaturate. “This newer and younger patient population is needing that home oxygen therapy,” she adds, “and that is something we have never really seen before.”
A form of post-COVID syndrome or “long COVID” is likely contributing to this need for home oxygen therapy in the younger demographic. LaRoche has been studying the matter and encountering more literature about so-called “fragility”—either genetically speaking or caused by asthma, hypertension, or diabetes. “Those patients are having this long COVID syndrome, or at least there is a higher instance of patients with those underlying conditions,” she said. “Those tend to be the people with long-COVID syndrome experiencing hypoxemia and significant shortness of breath. I don’t think we have a clean link just yet, but there also seems to be some connection between patients who are requiring oxygen post-COVID and being predisposed for heart disease and renal failure.”
Dunmire added that patients who are discharged with long-COVID symptoms are complex, and benefit from the added level of care that home ventilation provides. He explained that, “Home noninvasive ventilation programs typically include close follow-up with clinicians in the home and allow patients to be monitored carefully. In combination with advances in therapy, prognosis is typically good for these patients as they transition home and continue to heal in a subacute environment.”
High-flow Oxygen
For patients who need high-flow nasal cannula therapy at home, LaRoche maintains that the education portion is fortunately not that difficult. That said, the difficulty often comes via the device itself.
“The high-flow nasal cannula therapy devices are not super portable,” she said. “This is not like having an oxygen tank that you can roll around. If you are hooked to those kinds of devices, we can get you home but that does not necessarily mean you are going to be mobile as far as getting around and being outside. That’s a huge challenge for patients when bridging them out of the hospital.
“A lot of patients have done well using hi-flow nasal cannula, but we’ve had difficulty getting them weaned off of that fast flow, because it really satisfied their shortness of breath,” LaRoche continues. “People get dependent and we’re seeing a higher incidence of patients being stuck with the need for the therapy.”
Adaptive Therapies
As therapies continue to advance, ventilation trends include more adaptive algorithms as well as adjustments to how flow and pressure reaches the patient, mainly to prioritize patient comfort. Dunmire pointed out that with Movair’s Luisa home ventilator, high-flow therapy is offered as a secondary treatment mode. Patients can be managed with high quality ventilation via a mask at night and a high flow cannula during the day, bringing comfort to at-home recovery.
“Patients with chronic respiratory conditions including COPD and COVID-19 can be treated with a low-profile interface during the day to improve breathlessness and increase symptom control while also being able to eat, drink and participate in other activities of daily living,” Dunmire said. “The addition of high flow therapy for patients who qualify for home-based ventilation has helped to push the industry forward.”
While the profession progresses toward a normalization of the pandemic and fewer instances of ventilation, COVID is still very much top of mind among RTs. “You practice masked up,” LaRoche said. “Doing the work is still at a heightened level of safety, more so than it has been in the past. We are not anywhere near business as usual.”
NIV as a First Intervention Therapy
The events of the last two years have indeed made business as usual a distant memory for many RTs. Michael MacGregor, RRT, vice president of US sales for Bio-Med Devices Incorporated, Guilford, Conn., remembers the realization from hospital administrators who said, “We need ventilators like crazy.” And in the early days they did indeed put people on ventilators.
“There are two forms of noninvasive ventilation that would typically be a pre-cursor to the ventilator and that is a high flow nasal cannula system, and noninvasive ventilation like BiPAP,” MacGregor said. “But early on in COVID, they didn’t want to use those noninvasive modes because they felt there was no way to contain the virus if the exhaled gas went out into the air. So there was an early push to get people on the ventilator, and not on the noninvasive stuff. The problem was once COVID patients got on the ventilator, it was pretty much a 50-50 shot they were going to survive.”
Eventually pulmonologists realized that, “There really wasn’t this danger or threat of everybody catching COVID when they were on high-flow and noninvasive…For the patients, it was much better to keep them from being intubated. That was kind of the mode they tried to do with the high-flow and [NIV].”
With an eye toward the future, MacGregor reveals that Biomed’s newest ventilator, dubbed the TV-100 “actually has the high-flow nasal cannula function on it…It has the noninvasive function, and of course it has the full ventilator mode.”
“You also need to have a heated humidifier that humidifies the gas and heats it,” MacGregor adds. “You can’t send cold, dry gas to their nose. They’re not going to be comfortable. You must have a humidifier to go with that. It’s difficult to have a humidifier that you can actually roll down a hall, so we’re looking into putting something together that has a power supply on a stand with tanks and brackets—so providers could take patients who are on a high-flow cannula and take them to CT if they wanted to, or to X-ray…It’s something we’re looking into.”
Future COVID Care
Even with the forced evolution of ventilators over the past two years, LaRoche admitted, “I’m kind of a low tech person when it comes to ventilators.” Instead of technology that too often appears as “icing on the cake,” she favored the actual cake and hopes for more substantive additions in the future.
“I wish more ventilators had esophageal balloon monitoring,” LaRoche adds. “And if you want a wish list, I think a portable high-flow nasal cannula device would be great. If the industry wants to do something to help us, look into providing high-flow nasal cannula therapy out of the hospital, meaning in an ambulance for adults. Make devices so people can be more mobile in their home. That would be significant.”
RT
Greg Thompson is a contributing writer to RT. For more information, contact [email protected].