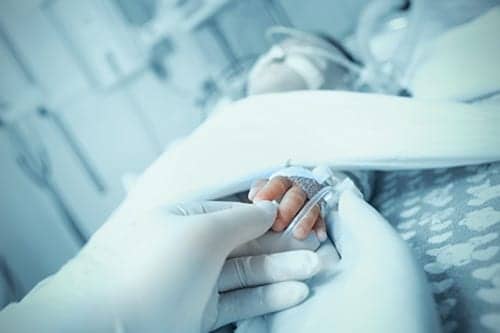
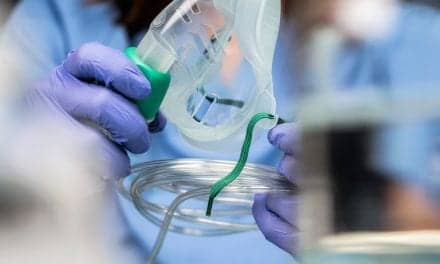
The technology for neonatal noninvasive monitoring is usually developed for the adult population and adapted for use in the newborn nursery. Thus, progress has been slow relative to developments in the adult field.
by John A. Wolfe, RRT, CPFT
Noninvasive monitoring of the newborn is a primal biological phenomenon, and many species within the animal kingdom monitor their offspring from birth. In medicine, touching and feeling were the first methods used; in more recent times, auscultation using a stethoscope and documentation of temperature via thermometer have provided important additional information. As medical knowledge has progressed exponentially, so has noninvasive monitoring.
Progress in neonatal monitoring has been slow relative to developments in adult monitoring, however. For most newborn noninvasive monitoring modalities, the technology has been developed for the wider adult population and is then adapted for the newborn nursery. There are three main reasons for this: neonatal medicine is a fairly new field, newborn monitoring requires miniaturization of existing technology and special designs because of the newborn’s unique physiology, and some manufacturers have been reluctant to invest in products that might produce a limited return.
Hospital and Home Monitors
One of the most basic requirements for the well-being of the newborn is a stable temperature. For premature and newborn infants, a neutral thermal environment should be maintained, with adequate warmth and humidity to minimize insensible heat and water loss.1 Temperature monitoring allows the caregiver to implement appropriate interventions to achieve thermal stability in the neonate. The temperature probe may be placed under the arm, on the infant’s abdomen, or in the rectum. It can not only monitor the infant’s temperature, but can connect to a radiant warmer bed and operate interactively to regulate the amount of warming. When the infant is too cool, the heat increases.
The first oximeters were expensive, cumbersome, cart-mounted devices with fist-sized, C-shaped probes and rubber ear covers. They failed to inspire confidence in clinicians who used them. Today’s pulse oximeters are now so ubiquitous, easy to use, and reliable that it is sometimes necessary to remind oneself to question or challenge the readings obtained from it. Although intended for adult use, the smallest pulse oximeters currently available are little larger than a clothespin, with both the electronics and light-emitting–diode windows integrated into the probe itself. Similar options for newborns cannot be far behind.
Neonatal pressure-cycled ventilators that provide minimal information about lung function are being replaced by much more sophisticated units that can be applied to adult, pediatric, or neonatal care and can provide a much better look at what the lungs are doing. Microprocessor technology built into the new generation of ventilators provides detailed monitoring parameters and alarm modes for patient spirometry, measuring tidal volume, minute volume, flow, compliance, airway resistance, and airway pressure. Liquid-crystal–display video monitors can add real-time pressure, flow, volume, and flow/volume loops. With pressure-regulated volume-control ventilation mode, for example, users can rely on the ventilator to adjust pressure automatically in response to changing lung compliance. While ventilator-based monitors could be considered invasive, no additional invasive technology is required for their use because the patient has already been intubated for ventilatory support.
Mainstream capnographs use a sampling window in the ventilator circuit to provide continuous analysis and recording of carbon dioxide levels in respiratory gases. Sidestream analyzers aspirate the gas from the circuit or a nasal catheter, and the analysis is performed within the monitor.2 In either case, clinicians are provided with important information about gas exchange. In addition, transcutaneous monitoring of oxygen and carbon dioxide provides estimates of PaO2 and PaCO2.3
For many years, apnea monitors have brought noninvasive monitoring of neonates into the home. Documented event monitoring simultaneously monitors three channels of information to provide monitor alarms or to verify the presence or absence of episodes of central apnea, bradycardia, and oxygen desaturation (events).5 Parents can care for their infants at home while continually monitoring chest-wall impedance, heart rate, and oxygen saturation.
Cardiac Output
Cardiac output can be extrapolated noninvasively based on respiratory gas analysis using a technique known as differential Fick partial rebreathing. An airway sensor, consisting of a rebreathing valve and a combined carbon dioxide/flow sensor, is placed in the breathing circuit. A noninvasive cardiac-output calculation is made based on the changes induced in carbon dioxide elimination and end-tidal carbon dioxide (etco2) in response to the rebreathing volume. The increase in etco2 reflects an increase in Paco2.
The Fick equation states that cardiac output is equal to carbon dioxide elimination divided by the difference between venous and arterial levels of carbon dioxide. The partial-rebreathing method yields a differential form of the Fick equation, eliminating the need to measure mixed venous carbon dioxide, so a pulmonary arterial line is not required as for the traditional (and highly invasive) thermodilution method. This indirect Fick method is then corrected for shunting, based on the Nunn isoshunt curve using oxygen saturation (from pulse oximetry or arterial blood-gas analysis) and a user-entered value for the fraction of inspired oxygen.4
This important tool for assessing and treating hemodynamic instability has not yet become the gold standard, and many clinicians maintain a trust-but-verify approach to it. Respiratory therapists may be seeking and developing evidence-based physician support. Studies are under way to document that, in real-world settings, calculating cardiac output noninvasively can reduce arterial blood-gas sampling, assist in optimizing ventilator parameters, assess weaning progress, and provide a reliable evaluation of the mechanically ventilated newborn.
On the Horizon
Today’s research and development teams are unveiling noninvasive monitoring techniques that no one would have been likely to imagine a decade ago. For example, a bilirubinometer that is effective in diagnosing and tracking jaundice using color-science technology has received clearance from the US Food and Drug Administration for commercial marketing. Soon, repeatedly drawing blood samples to assess bilirubin levels may become a practice from the dark ages of newborn care.6,7 Noninvasive monitoring for hemoglobin (hematocrit) using wavelength technology combined with a pressurizing site cuff is also in development.
Hospital personnel are constantly challenged by the ventilator tubing, intravenous lines, and monitor wires connected to critically ill patients. Parents may also be disturbed at the sight of their newborns tethered to so many devices. The challenge of noninvasive monitoring is compounded in the newborn nursery because of the tiny size of the patients. Clearly, it would be better to eliminate monitor wires without losing the important information that the monitors provide. An oximetry sensor, for example, could be powered by a miniature battery or solar cell and could transmit its information to a monitor mounted above the patient, to the nursing station, or to a handheld device carried by the RT.
Why settle for monitoring one or two parameters from a patch or probe? Why not incorporate many or all of the parameters to be monitored into one or two patches, or an elastic chest band, and eliminate most or all of the wires and cables? Research and development in the noninvasive-monitoring field are now focusing on incorporating wireless technology into current modalities and bringing diverse elements together in a cohesive package. When that becomes reality, it will be possible to monitor infants from any location, and the information generated will become part of the electronic medical record with no manual notation required.
This idea is currently in development throughout the industry, with devices built to measure several parameters not far behind. In Finland, for example, emergency medical technicians are reportedly using a monitor blanket that measures multiple parameters simultaneously. Although it is not available for use in the United States, and is not used for neonates, the concept is clearly far beyond the imagination stage. Refinement and implementation of similar technology can not be far away. As with most developments in newborn monitoring, breakthroughs are usually developed for the adult market and the technology is adapted for neonatal needs.
For about $100, bicyclists can purchase a wristwatch that monitors the rider’s current and maximum heart rate, exercise time, and information transmitted wirelessly from a sensor on the bicycle’s front fork, which is then used to calculate current, average, and maximum speed; distance traveled; and other trip data. The information can be downloaded to the cyclist’s computer wirelessly, as well. This device makes it obvious that most of the technology needed to integrate newborn monitors with life-support systems is already available to developers. Developments in artificial intelligence will also make it possible to evaluate and organize the data in a meaningful way. Clinicians could not only be warned of threatening conditions, for example, but specific plans of action could be suggested (and automatically enacted, if desired). A temperature probe is already trusted to adjust the heat lamp in a newborn’s bed. It is conceivable that clinicians will also come to trust other noninvasive monitors to interact with more sophisticated life-support systems, such as ventilators, to adjust settings within preset guidelines in reaction to changing patient conditions. The emerging field of microelectromechanical systems has important implications for the noninvasive monitoring and management of newborns, who will benefit from better monitoring, better life-support management, and more time with parents.
John A. Wolfe, RRT, CPFT, is a contributing writer for RT.
References
1. Fink JB, Hess DR. Humidity and aerosol therapy. In: Hess DR, MacIntyre NR, Mishoe SC, Galvin WF, Adams A, Saposnick AB, eds. Respiratory Care: Principles and Practices. Philadelphia: WB Saunders; 2002:635-635.
2. AARC Clinical Practice Guideline. Capnography/Capnometry During Mechanical Ventilation—2003 Revision & Update. Respir Care. 2003;48:534-537.
3. AARC Clinical Practice Guideline. Transcutaneous blood gas monitoring for neonatal and pediatric patients. Respir Care. 1994:39;1176-1179.
4. Estrem B. Infant apnea monitoring. In: Hess DR, MacIntyre NR, Mishoe SC, Galvin WF, Adams A, Saposnick AB, eds. Respiratory Care: Principles and Practices. Philadelphia: WB Saunders; 2002:550-564.
5. NICO Cardiopulmonary Management System User’s Manual. Wallingford, Conn: Respironics Novametrix; 2003.
6. US Food and Drug Administration Briefing Document for June 11 Open Session of the Pediatric Advisory Committee on Hyperbilirubinemia and Drug Development in the Term and Near–Term Newborn Infant. From: Division of Pediatric Drug Development; To: Pediatric Subcommittee of the Anti-Infective Drugs Advisory Committee. Rockville, Md: FDA; 2003.
7. Bertini G, Rubaltelli F. Non-invasive bilirubinometry in neonatal jaundice. Semin Neonatol. 2002;7:129-133.