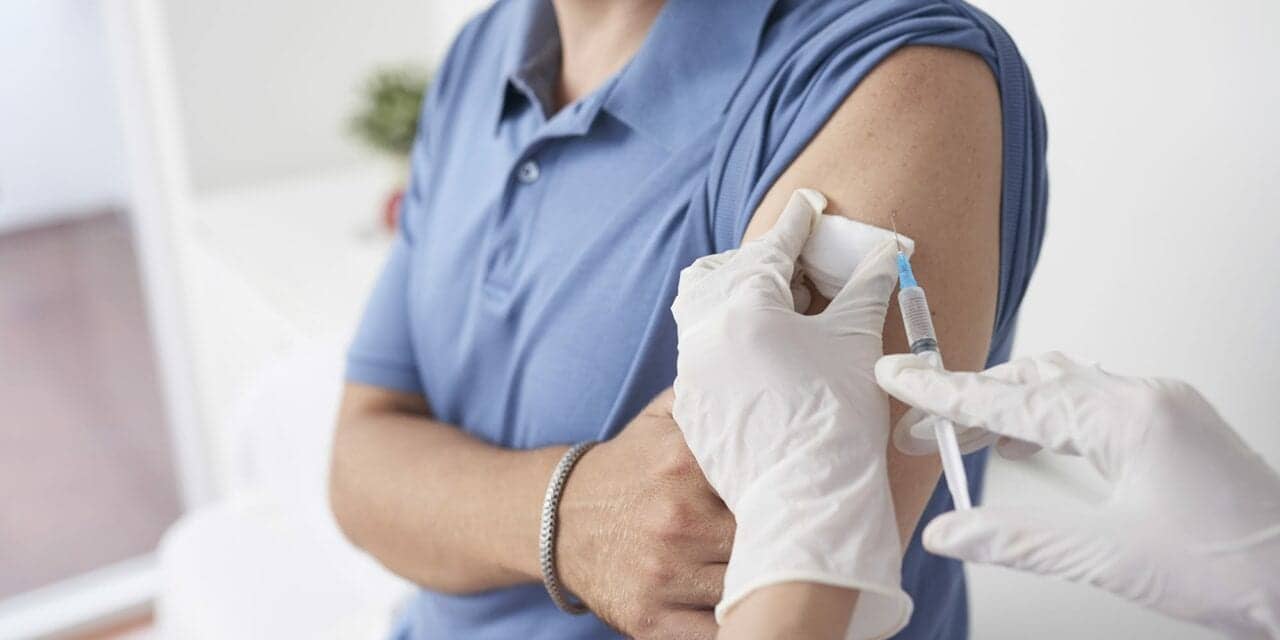
A homologous (same vaccine) booster of the J&J COVID-19 vaccine (Ad26.COV2.S) demonstrated 85% effectiveness against COVID-19-related hospitalization.
The study, conducted by the South African Medical Research Council (SAMRC), showed that the Johnson & Johnson booster reduced the risk of hospitalization from COVID-19 among healthcare workers in South Africa after Omicron became the dominant variant. During the months studied (mid-November to mid-December) the frequency of Omicron increased from 82 to 98 percent of COVID-19 cases in South Africa as reported by GISAID, an initiative that provides COVID-19 data.
A second, separate analysis of the immune response to different vaccine regimens, conducted by Beth Israel Deaconess Medical Center (BIDMC), demonstrated that a heterologous booster (different vaccine) of the J&J COVID-19 vaccine in individuals who initially received the BNT162b2 mRNA vaccine generated a 41-fold increase in neutralizing antibody responses by four weeks following the boost and a 5-fold increase in CD8+ T-cells to Omicron by two weeks. A homologous boost with BNT162b2 generated a 17-fold increase in neutralizing antibodies by four weeks following the boost and a 1.4-fold increase in CD8+ T-cells by two weeks.
The increase in CD8+ T-cells generated by the J&J COVID-19 vaccine may be key to explaining the high levels of effectiveness against severe COVID-19 disease and hospitalization in the Sisonke 2 study, as the Omicron variant has been shown to escape neutralizing antibodies.[1]
“Data from the Sisonke 2 study confirm that the Johnson & Johnson COVID-19 booster shot provides 85 percent effectiveness against hospitalization in areas where Omicron is dominant. This adds to our growing body of evidence which shows that the effectiveness of the Johnson & Johnson COVID-19 vaccine remains strong and stable over time, including against circulating variants such as Omicron and Delta,” said Mathai Mammen, M.D., Ph.D., Global Head, Janssen Research & Development, LLC, Johnson & Johnson. “We believe that the protection could be due to the robust T-cell responses induced by the Johnson & Johnson COVID-19 vaccine. Furthermore, these data suggest that Omicron is not affecting the T-cell responses generated by our vaccine.”
The data have been submitted to the pre-print server medRxiv by the studies’ authors, with anticipation of publication in peer-reviewed journals.
Phase 3b Sisonke 2 Booster Shot Study in South African Healthcare Workers
Data from the Sisonke 2 trial (n=227,310), conducted among healthcare workers in South Africa who received the single-shot Johnson & Johnson COVID-19 vaccine as a primary dose, show that the Johnson & Johnson COVID-19 booster increased vaccine effectiveness (VE) against hospitalization to 85 percent. When a booster shot was administered six to nine months after a primary single dose, VE increased over time from 63 percent (95% CI, 31-81%) at 0-13 days, to 84 percent (95% CI, 67-92%) at 14-27 days and 85 percent (95% CI, 54-95%) at 1-2 months post-boost.
Sisonke 2 was conducted in approximately 350 vaccination centers across all nine provinces of South Africa. Utilizing data from Discovery Health, a South African managed care organization, trial investigators determined VE of the Johnson & Johnson COVID-19 booster shot (n=69,092) as compared to other individuals enrolled in the same managed care organization, during the period from November 15, 2021, through December 20, 2021.
Enrollment for the Sisonke 2 arm of the trial commenced just prior to the onset of the Omicron wave in South Africa, allowing researchers to evaluate the effectiveness of the Company’s COVID-19 vaccine specifically as Omicron became the dominant variant in the country. Genomic characterization of isolates from COVID-19 cases was not conducted in this trial.
Healthcare workers have an increased risk of being infected with COVID-19, and in countries such as South Africa, which have a significant population living with comorbidities, the impacts of SARS-CoV-2 infections in healthcare workers are especially profound. The majority of South African healthcare workers who have died of COVID-19 had at least one comorbidity, and many had multiple comorbidities.
“Even before you factor in the increased infectiousness of Omicron, we have to remember that healthcare workers on the frontlines are at a greatly increased risk of being affected by COVID-19 in the first place,” said Glenda E. Gray, MBBCH, FCPaed (SA), President and CEO of the SAMRC. “We are therefore encouraged to see that boosting with the Johnson & Johnson COVID-19 vaccine regimen provides strong protection in a challenging real-world setting where there is an elevated risk of exposure – not just to COVID-19, but to the highly transmissible Omicron variant.”
Dr. Nicholas Crisp, the Deputy Director General of the South African National Department of Health said “The data showing the effectiveness of the Ad26.COV.2 vaccine booster against Omicron in Sisonke is important, as this vaccine is part of our arsenal to combat COVID-19. This data should reassure healthcare workers who have not taken their booster to get vaccinated as soon as possible.”
Antibody and T-Cell Responses After Heterologous Boosting Regimen Greater than After Homologous Regimen Against Omicron Variant
An analysis of 65 individuals who received primary vaccination with two doses of an mRNA COVID-19 vaccine (BNT162b2), followed by a homologous booster shot of BNT162b2 (n=24) or a heterologous booster with the Johnson & Johnson COVID-19 vaccine (n=41) after at least six months, found both regimens increased humoral and cellular responses against Omicron.
Antibody responses against Omicron were boosted by both the Johnson & Johnson COVID-19 vaccine and the BNT162b2 vaccine, with the Johnson & Johnson COVID-19 vaccine increasing neutralizing antibody titers by 41-fold at four weeks post-boost. The BNT162b2 vaccine was found to increase antibody titers to a higher level at week two post-boost, before declining to represent a 17-fold increase at week four post-boost. The progressive increase in antibodies the weeks following a vaccination of a Johnson & Johnson booster is similar to that seen following the first vaccine. The rapid immune response followed by waning of the antibody response after the BNT162b2 booster is also similar to that seen following the two-dose priming regimen.
The J&J COVID-19 vaccine boosted median Omicron-reactive CD8+ T-cells by 5.5-fold, and Omicron-reactive CD4+ T-cells by 3.1-fold, while the homologous (BNT162b2) regimen boosted both Omicron-reactive CD4+ and CD8+ T-cells by 1.4-fold.
T-cells can target and destroy cells infected by the virus that causes COVID-19 and are believed to contribute to protection against severe disease. Specifically, CD8+ T-cells can directly destroy infected cells and are aided by CD4+ T-cells.
These data suggest that heterologous boosting has the potential to induce strong cell-mediated immunity, which is important for immune memory and protection against severe lower respiratory tract disease. The durability of heterologous and homologous boost regimens for the SARS-CoV-2 Omicron variant remain to be determined.
“As the Omicron variant has mutated from the original SARS-CoV-2 strain, there is a need to understand how effective currently authorized COVID-19 vaccines remain at protecting against severe disease,” said Dan Barouch, M.D., Ph.D., Director of the Center for Virology and Vaccine Research at BIDMC. “Our analysis shows that a booster shot of the Johnson & Johnson COVID-19 vaccine generated a robust increase in both neutralizing antibodies and T-cells to Omicron.”