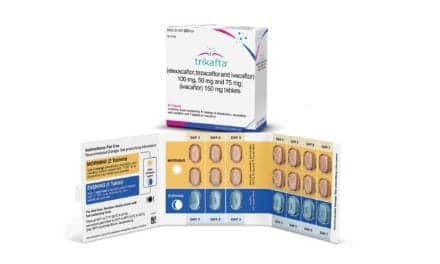
Probuphine, the first buprenorphine implant for the maintenance treatment of opioid dependence, has been approved by the US FDA. Probuphine is designed to provide a constant, low-level dose of buprenorphine for six months in patients who are already stable on low-to-moderate doses of other forms of buprenorphine, as part of a complete treatment program, the FDA said in an agency release.
Until today, buprenorphine for the treatment of opioid dependence was only approved as a pill or a film placed under the tongue or on the inside of a person’s cheek until it dissolved. While effective, a pill or film may be lost, forgotten or stolen.
However, as an implant, Probuphine provides a new treatment option for people in recovery who may value the unique benefits of a six-month implant compared to other forms of buprenorphine, such as the possibility of improved patient convenience from not needing to take medication on a daily basis. An independent FDA advisory committee supported the approval of Probuphine in a meeting held earlier this year.
“Opioid abuse and addiction have taken a devastating toll on American families. We must do everything we can to make new, innovative treatment options available that can help patients regain control over their lives,” said FDA Commissioner Robert M. Califf, MD. “Today’s approval provides the first-ever implantable option to support patients’ efforts to maintain treatment as part of their overall recovery program.”
Expanding the use and availability of medication-assisted treatment (MAT) options like buprenorphine is an important component of the FDA’s opioid action plan and one of three top priorities for the US Department of Health and Human Services’ Opioid Initiative aimed at reducing prescription opioid and heroin related overdose, death and dependence.
Probuphine consists of four, one-inch-long rods that are implanted under the skin on the inside of the upper arm and provide treatment for six months. Administering Probuphine requires specific training because it must be surgically inserted and removed. Only a healthcare provider who has completed the training and become certified through a restricted program called the Probuphine Risk Evaluation and Mitigation Strategy (REMS) program should insert and remove the implants, the FDA emphasized.
If further treatment is needed, new implants may be inserted in the opposite arm for one additional course of treatment. The FDA is requiring postmarketing studies to establish the safety and feasibility of placing the Probuphine implants for additional courses of treatment.
The safety and efficacy of Probuphine were demonstrated in a randomized clinical trial of adults who met the clinical criteria for opioid dependence and were considered stable after prior buprenorphine treatment. A response to MAT was measured by urine screening and self-reporting of illicit opioid use during the six month treatment period. Sixty-three percent of Probuphine-treated patients had no evidence of illicit opioid use throughout the six months of treatment – similar to the 64 percent of those who responded to sublingual (under the tongue) buprenorphine alone.
The most common side effects from treatment with Probuphine include implant-site pain, itching, and redness, as well as headache, depression, constipation, nausea, vomiting, back pain, toothache and oropharyngeal pain. The safety and efficacy of Probuphine have not been established in children or adolescents less than 16 years of age. Clinical studies of Probuphine did not include participants over the age of 65.