The National Institutes of Health has initiated a randomized, controlled clinical trial evaluating the safety and efficacy of the antiviral remdesivir (Gilead Sciences) plus the immunomodulator interferon beta-1a (Merck) in patients with COVID-19.
The study (Adaptive COVID-19 Treatment Trial 3, or ACTT 3), is anticipated to enroll more than 1,000 hospitalized adults with COVID-19 at as many as 100 sites in the United States and abroad.
Subcutaneous interferon beta-1a (marketed under the brand name Rebif by EMD Serono) is approved in the US and more than 90 other countries for the treatment of multiple sclerosis. The drug has the same amino acid sequence as a naturally occurring protein called interferon beta, which is part of a class of proteins called type 1 interferons. Infected cells normally produce type 1 interferons to help the immune system fight pathogens, especially viruses. Interferon beta has both antiviral and anti-inflammatory properties.
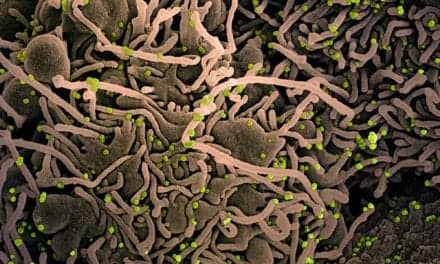
Laboratory studies suggest that the normal interferon response is suppressed in some people after infection with SARS-CoV-2, the virus that causes COVID-19. In the laboratory, type 1 interferon can inhibit SARS-CoV-2 and two closely related viruses, SARS-CoV and MERS-CoV. In addition, two small randomized controlled trials suggest that treatment with interferon beta may benefit patients with COVID-19. The combination of interferon beta-1a and remdesivir for treating COVID-19 has not been evaluated in a large, randomized controlled trial.
In accordance with standard clinical research protocols, eligible patients who provide informed consent will participate in ACTT 3. Participants must have laboratory-confirmed SARS-CoV-2 infection with evidence of lung involvement, including a need for supplemental oxygen, abnormal chest X-rays, or illness requiring mechanical ventilation. People with confirmed infection who have mild symptoms or no apparent symptoms will not be included in the study.
ACTT 3 participants are being randomly assigned in a 1-to-1 ratio to receive either subcutaneous interferon beta-1a plus remdesivir (combination therapy) or remdesivir alone. Neither the participants nor the study team will know who is receiving which treatment regimen. All participants will receive standard doses of remdesivir and either interferon beta-1a or a placebo. Those in the combination therapy group will receive interferon beta-1a as a 44-microgram subcutaneous injection every other day for a total of four doses during hospitalization. Those in the remdesivir-only group will receive a matching placebo subcutaneous injection every other day for a total of four doses during hospitalization.
Investigators will evaluate whether time to recovery is shorter in the combination therapy group relative to the remdesivir-only group. Recovery is defined as the participant being well enough for hospital discharge, meaning the participant either no longer requires supplemental oxygen or ongoing medical care in the hospital, or is no longer hospitalized (with or without some limitation on activities). Recovery is evaluated up until day 29. A key secondary goal of the study is to compare patient outcomes at day 15 using an ordinal eight-point scale ranging from fully recovered to death. The trial also will compare other secondary outcome variables between treatment groups, including mortality alone.
Preliminary results are expected in the fall of 2020, according to the NIH’s National Institute of Allergy and Infectious Diseases.