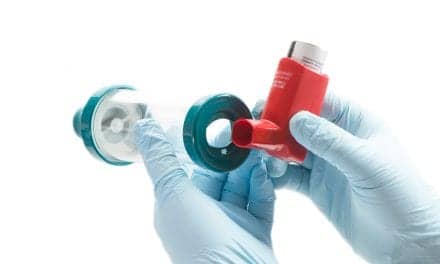
The oxygen device market is primed for growth and the quality of care for LTOT patients can benefit through innovative technology and appropriate services
 Long term oxygen therapy (LTOT) devices are evolving to a new level of sophistication. Equipment used for home oxygen therapy is being developed with the patient’s needs in mind, plus an appreciation for the costs associated with the service aspect of LTOT. This new breed of oxygen therapy equipment is arriving on the market at an opportune time since a large number of Baby Boomers needing LTOT are just starting to receive prescriptions for home oxygen therapy.
Long term oxygen therapy (LTOT) devices are evolving to a new level of sophistication. Equipment used for home oxygen therapy is being developed with the patient’s needs in mind, plus an appreciation for the costs associated with the service aspect of LTOT. This new breed of oxygen therapy equipment is arriving on the market at an opportune time since a large number of Baby Boomers needing LTOT are just starting to receive prescriptions for home oxygen therapy.
Historical Perspective
Less than 30 years ago, a prescription for home oxygen therapy would require an industrial gas supplier to deliver several large (H size) cylinders to a patient’s home. A large brass regulator would be put on the cylinder and a permanent humidifier attached for patient comfort. No portable systems were provided since oxygen therapy was prescribed at the end stage of the disease and the patients were typically bed-bound. This therapy would be provided for less than a year and in many cases only a few weeks.
The late 1970s brought a new concept to home oxygen therapy. A device was developed that could generate oxygen in the home and never need to be refilled. Oxygen concentrators became popular since they provided a convenience to the provider and unlimited oxygen to the patient. Portable oxygen was available as an emergency backup for the concentrator and could be used for short visits to the doctor or hospital. Patients were still not very ambulatory due to the progression of their disease and the lack of emphasis on activity. Liquid oxygen for home application was available and popular for patients who wanted to be active since the portable system was lightweight (compared to cylinders) and long-lasting. Liquid oxygen continued to grow in popularity as patients and physicians realized the advantages of exercise and pulmonary rehabilitation.
Two major changes have occurred over the past 20 years. Patients are being prescribed oxygen earlier in their disease and are younger and more active.
Younger, more active patients require an oxygen system that meets their needs for regular daily activity. Steel cylinders have evolved to aluminum and sizes have been shrinking to M6 cylinders holding 140 liters of gas down from E cylinders holding 680 liters. Oxygen conserving devices (OCD) have made the smaller cylinders more practical since the average 3:1 savings ratio allows for approximately 4 hours of mobility at a 2 lpm prescription.
OCDs have also helped liquid oxygen systems reduce size and last longer. A 3.5-pound liquid oxygen portable system can last for 8 to 10 hours at a 2 setting. These new liquid oxygen portables have rejuvenated the home liquid oxygen industry, and several manufacturers have introduced new small, lightweight portable systems
Clinical Research
Research has documented that oxygen therapy is effective in improving survival for chronically hypoxic patients. The NOTT study,1 published more than 20 years ago, indicated that continuous oxygen therapy improved survival over nocturnal oxygen therapy or no oxygen therapy. Two recent consensus conferences have focused on issues related to LTOT and attempted to outline solutions to the growing concern that federal reimbursement for LTOT is decreasing when demand is increasing.2,3 The general agreement is that oxygen is oxygen and whatever method used to delivery the oxygen should correct a patient’s hypoxemia. The consensus conferences and other research4 are beginning to evaluate and understand that the method of delivering oxygen has an impact on the patient’s ability to be active and mobile. Patients who exercise have fewer complications associated with their disease.5 It is generally understood that anyone, regardless of their disease state, maintains a better level of health if they exercise routinely. Oxygen systems that allow a patient to do activities of daily living will prevent complications and promote better health. Unfortunately, portable oxygen systems are more expensive to provide than stationary systems. Continued reductions in reimbursement for LTOT will challenge the ability of home care providers to give patients what they need and still operate a business profitably.
Evolution of the technology
Cylinders are now used as portable oxygen systems. Many patients still prefer an E cylinder as their portable since there is a safety factor of having enough oxygen available if the OCD should fail, plus they like the convenience of a wheeled cart that keeps the weight of the portable off their shoulders. Other patients like the M6 cylinder due to the small size and light weight. These systems can be placed in a case that hides the fact that they are using oxygen. Conserving devices make the small cylinders more practical since there would be minimal operating time with continuous flow.
Liquid oxygen is the most efficient method of storing oxygen. With an 860:1 ratio of gas to liquid, a very small amount of liquid oxygen can expand to a large amount of gas. Early liquid oxygen portables held 1 liter of liquid. Expanding to 860 liters of gas, a 9-pound liquid oxygen portable could provide more gas than an E cylinder at less weight. OCD on a liquid oxygen portable can reduce the amount of oxygen needed to provide the desired operating time, which is why the new generation of liquid oxygen portables are smaller, lighter, and longer-lasting.
Liquid oxygen base units have improved to reduce the normal evaporation rate (NER) and several systems have telemetry to allow for monitoring of content and schedule delivery.
 Figure 1. Comparison of a l liter liquid oxygen portable to an equivalent number of E size cylinders.
Figure 1. Comparison of a l liter liquid oxygen portable to an equivalent number of E size cylinders.
Concentrators have improved significantly in recent years. Systems currently on the market are more reliable at a lower cost and are the basis of most home oxygen therapy programs. Some manufacturers offer telemetry with their system, yet this technology has not been popular due to the additional cost and the lack of documentation as to why a provider would need the information.
Concentrators that fill portable cylinders are new to the market. The ability to fill a cylinder in the patient’s home gives the patient freedom to use as many cylinders as their lifestyle permits, plus the provider does not need to deliver cylinders to the patient’s home on a regular basis. Delivery of products to the home is one of the most expensive portions of a provider’s cost of LTOT services. The continued reductions in reimbursement from CMS have driven manufacturers and providers to focus on ways to reduce delivery expenses.
The purchase price of the home filling concentrator has been the barrier for providers to generally accept the system. A home filling system can cost up to three times the purchase price of a standard concentrator. The economics of eliminating the delivery of cylinders, the reduced inventory of cylinders, and accessories to support LTOT has not been clearly documented by independent research. Other issues of concern related to home filling concentrators is the additional cost of electricity that would be the responsibility of the patient, plus the issue of 93% oxygen from a cylinder filled by a concentrator. Cylinders are typically used during exercise and an OCD is utilized to extend operating time. The combination of 93% oxygen, an OCD, and increased respiratory rate has not been researched and might have an impact on the patient’s oxygen saturation.
A portable oxygen concentrator was just introduced to the market. Pending final Food and Drug Administration clearance, this unit will enter the market with claimed features of a 10-pound weight, 50 minutes of battery operating time, and 93% oxygen purity. The device will utilize an OCD and have five dose selection options. This unit will have the same challenges to market entry as the home filling systems with a higher cost and the issue of 93% oxygen delivered with an OCD to a patient with an increased respiratory rate. Clinicians have requested a portable oxygen concentrator for years and this new entry will start the process of refinement and improvement. Allowing one system to be the base unit and portable will further reduce the cost of LTOT and provide the independence patients are looking for from their oxygen system.
Oxygen conserving devices are one of the fastest growing areas of LTOT. Frost and Sullivan5 have estimated that the total number of OCD to be sold in 2001 is 129,971 and growing 15% annually. In 1984, the first intermittent flow oxygen delivery device was introduced to the home care market. In appreciation of the fact that oxygen delivered when the patient was exhaling was wasteful, this product sensed the patient’s inspiratory effort and delivered a dose of oxygen at the beginning of inhalation. This system eliminated the two-thirds of wasted oxygen that was being delivered during the patient’s exhalation and pause between breaths. Eliminating waste improved operating times and has been the basis for most new oxygen systems used in the home. Lightweight, long-lasting ambulatory oxygen is now possible to address a younger, active patient’s needs. An OCD can reduce the scheduled delivery of liquid oxygen and lower costs. New portable concentrators will depend on OCD technology to improve efficiencies and make lightweight concentrators possible.
Not all OCD operate the same. The method of delivery for different systems has been described as a pulse delivery, demand delivery, and hybrid.6 The method of delivery impacts the volume of oxygen that is provided to the patient. The volume per breath determines the FIO2 the patient is receiving at each setting. The settings on each OCD are reference points and should not be considered the same FIO2 as continuous flow or other OCDs at the same setting. This misconception was one of the reasons OCDs were not understood or used in the past due to poor patient oxygenation at a certain setting. Most patients can be oxygenated with an OCD if the setting is changed to meet their oxygen dose requirement. Saving ratio has been a claim of several manufacturers that believe their device performs better than others. The goal of oxygen therapy is to correct the patient’s hypoxemia. Once that goal is reached, the amount of oxygen saving can be a value. Withholding needed oxygen from a patient to improve saving ratio is illogical and dangerous. Most consensus conferences on LTOT recommend that a patient is tested on an OCD at each activity level and the appropriate setting selected to maintain oxygenation. This concept applies to all oxygen therapy, not just for conserving devices.
 Figure 2. Eight conserving devices set at 2 lpm. With increased respiratory rate, Fio2 varied between devices and continuous flow. Oxygen equivalency is a fallacy between continuous flow and different conserving devices.
Figure 2. Eight conserving devices set at 2 lpm. With increased respiratory rate, Fio2 varied between devices and continuous flow. Oxygen equivalency is a fallacy between continuous flow and different conserving devices.
Method of Oxygen Conservation
There are several methods of oxygen conservation. The most popular is intermittent oxygen delivery systems. Early generations of OCDs offered the conserving unit separate from the oxygen regulator. The first major breakthrough in the technology was a system that integrated the regulator with the conserving unit. This “doughnut”-style system had a cleaner presentation and convenience for the patient that requires changing the regulator when a cylinder is empty. The next breakthrough was the introduction of a pneumatic OCD. This simplified the system by eliminating the need to check and change batteries. The first pneumatic systems required a duel-lumen cannula to operate the device. These cannulas were a little more costly to the provider and heavier than basic cannulas for the patient. Cost and comfort have improved with new duel lumen cannulas. Just introduced was a single lumen pneumatic conserving device. A competitive market and research have stimulated the investigation of new and better ways to conserve oxygen. Again, with all the new technology being introduced, the first objective of oxygen therapy is to correct hypoxemia. The increased demand for effective, efficient LTOT devices will drive new products into the market. It will be the responsibility of the clinician to use these devices appropriately.
Patients
Patients are becoming active in teaching themselves about their disease and options for therapy. The Internet has provided a means for patients to search for information on their disease, network with others who have a similar disease, and review manufacturers’ Web sites for current technology. These patients are no longer dependent on their primary care physician or home care provider for answers to their questions. Options are now available to them and if they do not like the service they are provided related to LTOT, they search for better solutions. This patient “pull through” has stimulated the development of new oxygen systems that address a patient’s need for independence and mobility. New lightweight oxygen systems are selling because patients want them. These Baby Boomers are going to drive the development in oxygen products and services. If they do not get what they want under their insurance program, they may start paying for products and services out of their own pocket.
Conclusion
New lightweight oxygen systems are entering the market. New oxygen conserving devices are introduced every year. Options for reducing delivery costs associated with packaged oxygen are available with home fill concentrators: liquid oxygen-based units with conserving devices and the possibility of a concentrator filling portable liquid oxygen systems. A portable concentrator will enter the market next year and start the refinement on that concept. Baby Boomers are hitting the age where there will be the largest number of patients in that age bracket than has ever been experienced in the past. A new breed of patients is developing who know what they want and are seeking solutions to their health care needs. The oxygen device market is primed for growth and the quality of care for LTOT patients should be the best it has ever been with innovative technology and appropriate services.
Robert McCoy, BSM, RRT, is managing director of Valley Inspired Products LLC, Burnsville, Minn; www.inspiredrc.com.
References
1. Nocturnal Oxygen Therapy Trial Group. Continuous or nocturnal oxygen therapy in hypoxemic chronic obstructive lung disease: a clinical trial. Ann Intern Med. 1980;93:391-398.
2. Petty TL, Casaburi R. Recommendations of the Fifth Oxygen Consensus Conference. Writing and Organizing Committees. Respir Care. 2000;45:957-961.
3. MacIntyre NR. Long-term oxygen therapy: conference summary. Respir Care. 2000;45:237-245.
4. Petty TL, Bliss PL. Ambulatory oxygen therapy, exercise, and survival with advanced chronic obstructive pulmonary disease (the Nocturnal Oxygen Therapy Trial revisited). Respir Care. 2000;45:204-211.
5. Frost & Sullivan. US Oxygen Therapy Device Markets. Mountain View, Calif: 1999.
6. McCoy R. Oxygen-conserving tech-niques and devices. Respir Care. 2000;
45:95-103.