As telemedicine opportunities expand, companies and respiratory care professionals are developing mobile health devices that connect more patients with the benefits of pulse oximetry.
By Phyllis Hanlon
In healthcare, electronic information exchange between patients and hospitals and physicians is becoming a more common and acceptable form of communication. Electronically transmitting vital signs and other health indicators, such as blood glucose levels and heart echocardiogram readings, has several advantages over traditional patient monitoring methods. Forty years ago, physicians had to see patients in the office to collect health information.
Today, telemedicine, the exchange of medical information from one site to another via an electronic communication system, is reducing the number of office visits a patient is required to make, while appropriately monitoring health conditions. One of the tools making notable strides in the high-tech arena is the pulse oximeter.
Effective Patient Management
Mark VanderWerf, vice president of eHealth and OEM at Nonin Medical Inc, explained, “In the past, we might depend on the patient to record their readings manually and save them for later discussion with caregivers. This resulted in errors and the information was usually too old to be of use.
“With a wireless radio, the patient measurement is captured automatically without error and is sent immediately. The systems that receive the information can see changes and alert caregivers as needed. This allows for very effective patient management as well as greater comfort and independence for the patient.”
VanderWerf added, “When managing patients with disease, it is critical to know about changes in condition. This requires accurate, consistent measurements. Failure to see changes can result in a failure to intervene, which can lead to an acute event and an often unneeded hospitalization.”
Bluetooth Technology
Since 1986, Nonin Medical has manufactured pulse oximeters and recently developed several wireless models. Nonin’s WristOx2 Model 3150, a wearable pulse oximeter, uses Classic Bluetooth radio to measure oxygen saturation levels continuously. The device utilizes PureSAT pulse-by-pulse filtering that provides precise measurements despite motion, low perfusion, or other adverse conditions.1
“It records the changes in a patient’s pulse and oxygen saturation over a prolonged period, or multiple periods, usually overnight,” VanderWerf explained.
When the patient wakes in the morning and removes the device, the stored information is sent to an independent diagnostic testing facility or healthcare provider, where an appropriate course of action is determined. All transmitted data complies with privacy and security regulations, contains no patient identifiers, and can be encrypted, which makes it unreadable, noted VanderWerf.
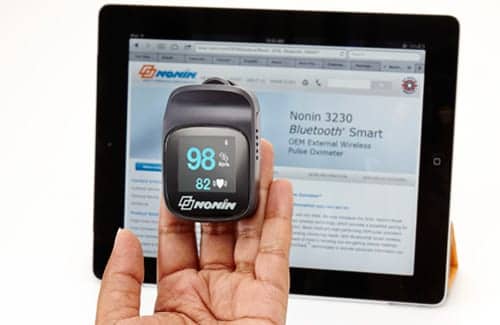
The Onyx II Model 9560, the first finger pulse oximeter to use Bluetooth technology to transmit information wirelessly, takes a discrete measurement at a point in time versus continuous measurements. The device turns on when the patient inserts his finger and, when it captures a good measurement, automatically sends the data to a telehealth system or a data hub in the home and turns itself off.
Advanced Bluetooth
One of the newest devices is the “Smart” finger pulse oximeter, the first to incorporate Bluetooth Smart (low energy) wireless technology. Nonin Medical 3230, which is designed for a variety of telehealth installations for patients with chronic obstructive pulmonary disease (COPD), congestive heart failure (CHF), asthma, and other chronic illnesses, has received clearance from the Food and Drug Administration (FDA).
“Almost all mobile device makers began to build Bluetooth Smart into their smartphones, tablets, palm devices, and laptops mid-last year. This opens up a wide new universe of devices that Bluetooth Smart can connect to, including iOS devices, which needed an authentication chip to work with Bluetooth Classic,” said VanderWerf.
Although a groundbreaking technology, Bluetooth Classic had difficulty syncing with other devices.
“This required the entry of unique identifiers in advance. A secondary challenge was patient use. Last generation devices had a fairly basic interface,” VanderWerf said. “The new 3230 with Bluetooth Smart overcomes both these challenges and supports ‘simplified pairing.’ This allows the device and the system to pair automatically. The 3230 also has a richer user interface. The screen is large and clear. Nonin’s graphic interface guides the patient in proper use of the device.”
VanderWerf added that Bluetooth Smart uses only a fraction of the power of Bluetooth Classic, so battery life is extended and implementation costs are much less. “We believe its ease of use and reduced cost will make it more attractive for more personal use applications,” he said.
To ensure proper usage of these pulse oximeters, Nonin developed CorrectCheck, a digital display that instructs the patient on the appropriate way to apply the oximeter. “If the finger is not inserted properly, it would lead to a false, imperfect reading,” VanderWerf said.
Healthy Applications
Nonin’s finger pulse oximeter is fully interfaced with IdeaSynthesis LLC’s SimpleEye Modern Mobile Health Solutions (Boston). The engineer behind the software, Femi Omojola, said he developed SimpleEye after realizing that postoperative care fell far short of what he considered appropriate.
The application he created is meant to serve as a long-term monitoring tool, both for post-op patients and for individuals with COPD or other lung conditions.
“The data gets uploaded automatically to the electronic health record. The doctor could read it and monitor the person’s health condition and make changes when appropriate,” Omojola explained. “The idea behind the app is to make taking pulse oximetry readings a habit.”
The data consumes very little space, and 2- to 3-year-old smartphones have plenty of storage capacity, according to Omojola. “You could take two measurements every day for the rest of your life and store it. The data never goes away. From a tooling perspective, it has a simple display and easily exports data to Excel.” The app relies on data provided by clinical grade, FDA approved and supported devices, Omojola reported.
Phone Oximetry
J. Mark Ansermino, MBBCh, MMed, MSc, associate professor of anesthesiology and director of pediatric anesthesia research at British Columbia’s Children’s Hospital (BCCH) in Vancouver, Canada, noted that, although pulse oximeters are fairly simple, they had not been taken out of the operating room due to the high cost of implementation.
Using smartphone technology, Ansermino hopes to make pulse oximetry widely available in the community, as well as in geographically remote areas where pulse oximetry is unavailable during procedures involving anesthesia.2
In 2009, Ansermino and his colleagues formed Lionsgate Technologies (LGTmedical)—an mHealth spinoff out of the University of British Columbia, BCCH, and the Child & Family Institute—and sought first-round financing to conduct further research for their Phone Oximeter project.
Determined to “put a pulse oximeter in every home” at a reasonable cost, Ansermino and his team examined the use of a closed loop control system that would enable a pulse oximeter to work on a cell phone.
“We thought if we could plug in the pulse oximeter, it would reduce costs. We had some ideas, but they still cost a few hundred dollars. You still had to have a pulse ox processor, inline cable, or something else,” he said. “We also looked at using the sound card of a cell phone. It would be like taking an analog signal and converting it to a digitized signal. We decided to get rid of the external device and use the audio jack, which is available on any cell phone.”
During initial research efforts, Ansermino faced several stumbling blocks, mostly related to the quality of the product. “You can buy a pulse oximeter for $20, but it’s unlikely to produce numbers you can have confidence in,” he said, adding that he wanted to create a product that resembled those manufactured by Masimo, which he feels is the “gold standard.”
The first iteration of the Phone Oximeter is designed for use only on the iPhone, iPad, and iPod Touch. “Later ones will work for Android and then Blackberry,” Ansermino said.
Accuracy and Usability Studies
Ansermino has conducted and published several studies on the Phone Oximeter’s accuracy, which, for the most part, comes close to that found in Masimo products, he claimed, except in patients in low perfusion states.
A 2012 study assessed the usability of the Phone Oximeter by evaluating the ease with which users with variable pulse oximetry and mobile phone experience were able to execute a series of interactive tasks with the device.2
Phase One of the study included 20 participants, nine of whom (43%) had never used smartphones with multitouch capability. The other 11 participants had been exposed to or had regularly used this type of device. All participants had extensive prior experience with pulse oximetry. The findings indicated that the prototype Phone Oximeter was very usable both by medical staff in a developed world setting and by a range of anesthesiologists and medical care providers in the developing world.
During the testing of the first prototype Phone Oximeter in Canada, the researchers identified specific failings in the interface design. In addition to developing an interface that would be easy to master for expert and less experienced users, Ansermino and his team wanted the interface to be language-independent. They made improvements, which reduced the number of errors in a subsequent trial that took place in Uganda, even though the users in this study were generally less experienced medical personnel.
Feedback from study participants was very encouraging, and participants, despite encountering some areas of difficulty, embraced the concept unanimously, according to Ansermino.
The findings of this usability study demonstrated that a fully functional interface could be implemented on a mobile phone-sized screen without losing the practical usefulness of standard pulse oximetry. Familiarity with the use of mobile phones or pulse oximeters did not significantly influence performance during testing.
Currently, 77,000 operating rooms worldwide do not have pulse oximetry, according to Ansermino, and he believes the Phone Oximeter could be a link in bridging this deficiency gap. The Phone Oximeter has the ability to complement existing global healthcare strategies, such as the Mobile Medic Program in Malawi,4 an international mHealth project designed to assist clinicians in improving care for patients with communicative and geographic barriers by eliminating long-distant trips in favor of telemedicine.
Ansermino believes the Phone Oximeter’s built-in mobile phone compatibility will help community workers make better decisions regarding treatment options or referrals; in remote geographic areas, healthcare workers will be better equipped to respond more appropriately when immediate clinical support is not available.
Benefits for Multiple Populations
With regard to the utility of the Phone Oximeter, Ansermino foresees benefits for children, pregnant women, those with respiratory conditions, and airline passengers. The device could help detect preeclampsia, Ansermino said, a condition that can increase the risk of stroke and/or seizures in pregnant women and affects every system in the body, including the lungs.
The World Health Organization (WHO) reports that approximately 500,000 women—many from developing countries—die each year from pregnancy-related complications. Women in African and Asian countries may develop hemorrhage, hypertension, obstructed labor and/or septicemia; delays in diagnosis, triage, transportation, and treatment can complicate the situation.3
“Ten percent of women get this, and a small percentage develop severe life-threatening complications. With the Phone Oximeter, you could figure this out ahead of time and avoid complications,” Ansermino noted. “A study showed that most women who develop complications have low O2 saturation. Pulse oximetry could be a predictive tool.”
Altitude affects oxygen levels so Ansermino sees some benefit for patients with respiratory conditions or using supplemental oxygen traveling by airline. “Everyone who gets on an airplane could use the Phone Oximeter. If your pulmonary function is not good, your oxygen level is not good,” he said.
Additionally, the device would be a more convenient way to screen for obstructive sleep apnea compared to a typical polysomnography test, which can require an inpatient stay of 24 hours. “The Phone Oximeter could be used as a screening tool to see who has to come into the clinic for the next step. Overnight oximetry [at home] would eliminate the hospitalization piece,” Ansermino said.
Industry Standards
A few agencies are collaborating to standardize interoperability guidelines for mobile-integrated pulse oximetry. One of these agencies, the Continua Health Alliance, a 200-member, nonprofit industry coalition launched in 2006, is working with IEEE, which has established a well-defined model on how to improve interoperability between pulse oximeters and cell phones, handsets, tablets, smart personal devices, and other electronic devices, according to Continua’s executive director Chuck Parker.
“These devices are designed for use outside the clinical setting, specifically in long-term care facilities and home settings. We aim to make them highly usable and portable and reduce the technological aspect for the user. We want to make it simple for the individual to get information to the care team and integrate devices so it’s easier to collect data.”
Although Continua’s member companies are working toward the same goal, convincing all parties to agree to all standards is, at times, somewhat challenging. “They are beginning to understand the best model, so now it’s a matter of getting them to agree to the final details,” said Parker. “Another challenge is breaking down the barriers around proprietary architecture. Companies use this as a way to lock people into using their solution.”
These barriers, however, may soon crumble. Parker reported that Denmark and Singapore now require interoperability for all medical devices. He does not anticipate that the United States will mandate interoperability, but believes the government will recommend flexibility in existing standards.
“This means you could build one device and sell it anywhere. The standards wouldn’t change because they are being used in a different country,” Parker said. With 4 billion mobile phones currently in use—and the number continually growing—the biggest question will be network capability. The flood of information may overwhelm an inadequate system, added Parker.
Integrating the Healthcare Enterprise—Patient Care Device Domain (IHE-PCD) concentrates on interoperability with the electronic health record (EHR). Created in 2005, this domain also uses IEEE 11073 as its information model. Unlike Continua, which tests devices through a certification process, IHE-PCD conducts “Connectathons” that assess whether a vendor has conformed to the standards.
The American Society for Testing and Materials (ASTM) with cosponsor American Society for Anesthesiologists (ASA) commissioned the Integrated Clinical Environment (ICE) standard, a medical system designed to safely acquire and integrate data between devices from patients in high-acuity environments. This standard requires a point-of-care system that incorporates patient safety, treatment efficacy, and workflow efficiency in biomedical devices.
The US Department of Health and Human Services (HHS) has chartered the Health Information Technology Standards Panel (HITSP) to standardize health information technology compliance with the federal mandate for electronic health records. HITSP developed interoperability specifications, to which all contributors to an EHR must adhere. HITSP recommends remote monitoring medical device interoperability be available by 2013 or 2015.
Technology is virtually shrinking the size of the global community. As more advanced wireless devices with the ability to communicate with other electronic tools are brought to market, post-op patients, individuals with respiratory illnesses and other chronic conditions, as well as their healthcare providers will reap significant medical benefits. RT
Phyllis Hanlon is a contributing writer for RT. For more information, contact [email protected].
References
- 1. http://www.nonin.com/documents/8729-001-01%20PureSAT%20Accuracy%20in%20Motion.pdf
- 2. Hudson J, Nguku SM, Sleiman J, et al. Usability testing of a prototype Phone Oximeter with healthcare providers in high- and low-medical resource environments. Anaesthesia. 2012;67:957-967.
- 3. http://pre-empt.cfri.ca/Portals/0/MaternalOutcomes-miniPIERS_20110125.pdf
- 4. Mahmud N, Rodriguez J, Nesbit J. A text message-based intervention to bridge the healthcare communication gap in the rural developing world. Technol Health Care. 2010;18(2):137-44.