Respiratory compromise affects thousands of patients every year, resulting in frequent intubations, high mortality rates, increased hospital stays, and billions in healthcare spending.
Respiratory compromise, defined by Medtronic as the cascade from respiratory distress to insufficiency, arrest and finally failure, continues to top of the list of costly conditions in US hospitals. In 2007, respiratory compromise was related to 385,800 inpatient stays and carry a price tag of $7.7 billion. A 2010 statistical brief from the Agency for Healthcare Research and Quality (AHRQ) reported that respiratory insufficiency, arrest and failure are three of five conditions that account for the high costs of Medicare-covered hospital stays.1
By 2019, the cost of inpatient stays associated with respiratory compromise is expected to surpass $37 billion.2 Moreover, Medicare’s Inpatient Quality Reporting Program (Patient Safety Indicator #11)3 focuses on postoperative respiratory failure and asserts that current monitoring regimes fall short when it comes to preventing respiratory compromise.
From Single to Multiparameter Devices
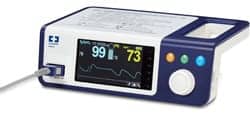
Certain standalone devices, such as the pulse oximeter, continue to be a first-line monitoring tool for both inpatients and outpatients. Mark Goldberg, product marketing manager for the Fingertip Division at Nonin Medical Inc explained that the pulse oximeter offers the patient and clinician a clear picture of oxygenation. “It’s one of the key measures for knowing the patient is doing okay,” he said. “[Outpatients] can use the pulse oximeter to track improvement. It provides a metric to know how well they are managing their condition,” he said.
For instance, a wrist model monitors oxygenation during six-minute walk distance (6MWD) testing and during overnight sleep studies, while a table top model is applicable for spot checking as well as continuous monitoring of blood oxygen saturation and pulse rate for patients from neonates to adults.
Goldberg noted that during transport a handheld oximeter or a fingertip model tracks changes in peripheral oxygen saturation (SpO2). “The handheld and fingertip models can also monitor patients in the waiting room,” he said. “When a multi-parameter device is not available, it’s easier to pull a pulse oximeter out of your pocket and put it on the patient.”
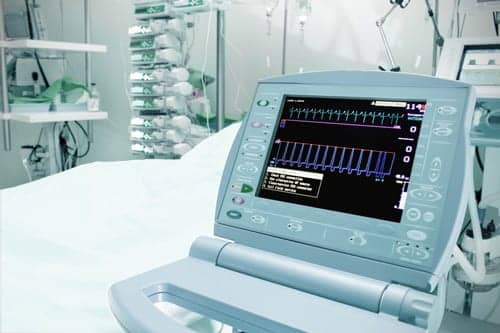
When integrated into a multi-parameter device, the oximeter works as part of a larger overall monitoring solution. For instance, during procedural sedation, opioid pain management administration and sleep studies, a combination pulse oximeter and capnograph monitors SpO2 as well as end tidal carbon dioxide (EtCO2). “Capnography provides a faster read on the patient’s O2 level. There is a 20 to 30 second delayed reading from the heart to the finger. You need to know faster if the patient’s O2 level is okay,” Goldberg said. “Many multi-parameter devices use the Nonin pulse oximeter. It’s about enabling the multi-parameter device manufacturer to provide pulse oximetry without taking up a lot of space and requiring a lot of power.”
Goldberg pointed out that multiparameter devices also interface with the patient’s electronic medical record and typically are equipped with alarms that alert nursing staff to a possible medical issue.
Continuous Monitoring
Respiratory compromise can occur at any time during an inpatient stay. But Brian Carlin, MD, a contractual pulmonologist at PA Critical Care Associates, reported that this event doesn’t typically happen in the intensive care unit (ICU). “We watch them pretty closely in the medical ICU,” he said, pointing out that the nurse/patient ratio is usually 1:3. “On the general medical floors it’s more common to see respiratory compromise. Patients are sicker than the doctor may realize or may have multiple comorbid illnesses. The patient is given analgesics, anxiolytics or insomnia medications that may cause respiratory compromise.” Floor nursing staff often has a patient load of eight to 10.
Patients with comorbid conditions such as sleep apnea and chronic obstructive pulmonary disease (COPD), which are sometimes undetected, require careful monitoring when given a combination of pain and sleep medication. Monitoring older patients is also critical since they are often given a standard medication dose. “Age affects the way the body metabolizes medication,” said Carlin.
The advent of new integrated capnography/oximetry devices have been “very helpful for patients on narcotics,” according to Carlin. “Now, even if there is a whiff of sleep apnea, hospitals put patients on a monitor. Hospitals are more aware and have created protocols,” he said, adding that on the general floor the devices can ward off the need to intubate. “You want to prevent [intubation] before it presents its own cascade of events.”
Educating the Clinician
In addition to distinguishing between ICU and general floor patients, Philip Porte, executive director of the Respiratory Compromise Institute (RCI), separates medical from surgical patients. Response on the medical floor is typically reactive, while in surgery, proactive responses are the norm, he asserts and suggests that health care practitioners need to understand indicators potentially leading to mechanical ventilation. “When I worked in pulmonary critical care, the doctors would deal with respiratory compromise after the accident happens. They know about COPD, but if the patient has diabetes or another medical history, they don’t know enough yet to make a judgment,” he said. “RCI broadened our advisory committee to include other specialties. We’re getting a clearer picture of what needs to happen to reduce respiratory compromise.”
Additionally, physicians should examine exactly what measures are being monitored to maximize efficiency. “Are there aspects of the patient that we don’t need to monitor?” Porte said. “Practitioners and hospitals need to be educated. It’s not as simple as ‘everyone needs it.’ We have to identify those at high risk. Across the medical spectrum there are patients who might be moving downward in a respiratory cascade.”
RCI recently finished a significant Medicare data mining project to get a better idea of the scope of the problem. “The premise was to look at claims for patients where respiratory failure was not present on admission,” he said. “Respiratory compromise doesn’t appear much in medical literature so we struggle to do meta analyses.”
Return on Investment
Studies have found that patient monitoring, specifically continuous monitoring, is associated with a marked decrease in length of stay, in ICU days for transferred patients and in code blue rates4 and provides a positive return on investment (ROI).5
Tim O’Malley, president, EarlySense Inc, explained that a nurse managing four or more patients can capture only so many data points to make clinical assessments regarding pain, sepsis, respiratory status and other medical conditions. To maximize clinical efficiency and patient safety, EarlySense’s All-in-One, a non-invasive device, captures as many as 60,000 data points every four hours and analyzes the information. “The device can detect potential respiratory depression and send an alert to the caregiver through the bedside monitor to the central station and to a mobile device,” said O’Malley. “It monitors up to 40 patients simultaneously. Measuring respiratory rate is a challenge. Clinicians look at the chart and the respiratory rate looks relatively stable. But we have the science behind [this technology] so [capturing multiple data points] becomes a big advantage.”
O’Malley explained that sensors, the size of a pad of paper, are placed underneath the mattress and absorb signals from the body. “Behind the scenes, algorithms are computing the waveform data. There is a lot of computation going on in the background, looking at respiratory rate, the leading indicator of respiratory compromise. We simplify it as a number on the screen,” he said. “There is also a trend screen that looks at the rate of days or hours. If the patient is deteriorating, the clinician will see it.”
As far as costs are concerned, a device that captures numerous data points on a continuous basis has a measured clinical impact on the patient, shortening time in the ICU and reducing code blue rates by more than 80%.4 “It’s one thing to save money, but CFOs want to see hard money. They want to generate increased revenue and [can do that] because of savings on the length of stay. Bed availability becomes greater,” said O’Malley. “As an industry we have to have a multi-faceted approach to provide clinical outcomes, return on investment and generate revenue.”
Changing a Culture
Sam Ajizian, vice president, Medical Affairs, Medical Director and Safety Officer, Patient Monitoring and Recovery at Medtronic, reiterated that monitoring the patient can help identify sentinel events early and advocates for continuous monitoring to ensure patient safety. He said, “[Continuous monitoring] shifts across a continuum from initial status to respiratory arrest and gives good evidence how to triage the patient.”
Practitioners, however, must be proactive, not just reactive, in monitoring patients. “We need to transfer vigilance into prospective monitoring for those patients at risk so we can intervene early,” he said, adding that the available resources in a medical facility will dictate when to begin monitoring.
When you make a concerted effort to reduce respiratory compromise, it comes with a responsibility to create a culture within the staff that understands and knows how to utilize technology, according to Ajizian. “Putting the patient on a monitor is not enough. Coupling the device technology with long-term support will ensure proper deployment and implementation,” he reported, but noted that getting clinicians to use the devices can be challenging. “I’ve seen countless devices gathering dust in a corner. The patient won’t benefit if the device isn’t used properly. It’s impossible without education to change the culture. This is related to the non-sustainable nature of medical devices without support.”
Medtronic partners with its customer institutions to create a proper system for their unique needs and offers training on an ongoing basis. Ajizian said, “Every hospital is different and every patient population is different. One of the strengths at Medtronic is that we invest the time. We offer suggestions and guide them through the literature on how to manage alarms.”
In the course of educating a customer institution, Medtronic identifies the hospital’s expectations and key stakeholders. “We also ask if the hospital is increasing monitoring based on several sentinel events or as part of a proactive process,” said Ajizian. Medtronic examines the culture at the facility and completes a full assessment of the patient population, skill level of the providers, ratio of staffing to patients and commitment of administration to sustain efforts. “We’ve created an ‘Outcomes pledge,’ which are long-term agreements to improve certain metrics,” Ajizian said.
According to Ajizian, respiratory therapists welcome new integrated monitoring devices. “Hospitals have shorter staffing in ward spaces and respiratory therapists embrace any technology that is easy to use, while providing a sustainable and accurate early warning. It empowers the RT to do his or her job better and keep the patient safer.” RT
Phyllis Hanlon is a contributing writer to RT. For further information, contact [email protected]
References
-
Wier LM, Henke R, Friedman B. “Diagnostic Groups with Rapidly Increasing Cost, by Payer, 2001-2007: Statistical Brief #91.” Healthcare Cost and Utilization Project (HCUP) Statistical Briefs. Rockville, MD 2010.
-
Agarwal SJ, Erslon MG, Bloom JD. “Projected incidence and cost of respiratory failure, insufficiency and arrest in Medicare population, 2019.” Abstract presented at Academy Health Congress, June 2011.
-
Zhan C, Miller MR. “Excess length of stay, charges, and mortality attributable to medical injuries during hospitalization.” JAMA. 2003;290(14): 1868-1874.
-
Brown H, Terrence J, Vasquez P, et al. “Continuous monitoring in an inpatient medical-surgical unit: a controlled clinical trial.” Am J Med. 2014;127(3): 226-232.
-
Slight SP, Franz C, Olugbile M, et al. “The return on investment of implementing a continuous monitoring system in general medical-surgical units.” Crit Care Med. 2014. Aug;42(8): 1862-8. doi. 10.1097/CCM.0000000000000340.