|
Home is where the heart is. And, increasingly, the lungs.
Thanks to modern technology coupled with more enlightened thinking among payors, growing numbers of ventilator-dependent patients are spending their days and nights in the familiar, comfortable confines of their own domiciles. No longer is their only option a protracted stay in the hospital or even consignment to a long-term care facility.
Home, many now agree, is generally better for patients but only if the clinical and caregiver support they receive there is adequate. As many providers of home mechanical ventilation have discovered, there exist challenges aplenty to giving ventilator patients what they need for success outside the institutional setting. For instance, studies show that home ventilator caregivers suffer significantly higher rates of depression than the societal norm—and a roiled psyche is far from the ideal state of mind for one to be in when attending so involved a patient, suggests Angela King, RPFT, RRT, NPS, Spencerville, Ind-based vice president of clinical services and clinical marketing for Breathe Technologies, Fremont, Calif.
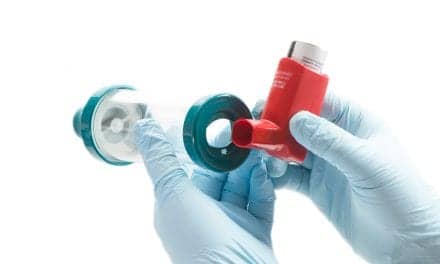
Depression can be fueled by information and sensory overload, she adds. “The demands of caregiving are relentless in some situations, and a ventilator is just the start of things,” says King, explaining that the homes of machine-dependent patients not infrequently end up mirroring a hospital intensive care unit for sheer number of systems, supplies, and medications, all of which must be intimately understood by the family and friends tapped to serve as caregivers. “There could be a primary ventilator at the bedside, a portable ventilator on the wheelchair, batteries and chargers for both, a line heater-humidifier, an oximeter, a stationary and a portable suction machine, two types of oxygen systems, a nebulizer and, often, a feeding pump as well. And that’s just the equipment. Then there are the supplies. Trach tubes, cannulas, suction catheters, the list goes on and on. It is by no means easy for individuals without clinical orientation or training to monitor and manage these many items.”
What is easy is seeing how this responsibility could overwhelm and cause emotional difficulties.
Short-Changed, Short-Staffed
Another challenge to providing mechanical ventilation in the home is, as always, reimbursement. In a nutshell, payment offered by Medicare and private insurers can affect the choice of ventilator supplied for home use. Says King, “Reimbursement may be deficient to the point that a DME [durable medical equipment] provider can’t justify carrying the latest and greatest in equipment.” Meaning, the patient might receive second best. Or third best.
Reimbursement also impacts the number of circuits and supplies to which a home ventilator patient is entitled monthly. Financial limits on those items can affect clinical care, King warns. “If you’re not allowed an adequate number of circuits, for instance, you’ll end up stretching the use of each one so that your allotment won’t run out before your next resupply,” she says. “But if you use circuits and other tubes beyond a certain point, their performance may be reduced due to the presence of pinholes or the loss of integrity of the material. Plus, you can have bacteriologic issues.”
 |
| Adhering closely to insurer-supplied medical necessity guidelines is important, as is submitting proper documentation. |
Being shorted on reimbursement is one problem. Being shorted on clinical staff for home visits and assessments is another. As King points out, visits from nurses are beneficial to home ventilator patients. Payors understand this, and so they often allot a certain number of hours per month for nurse visits, but nurses are hard to come by these days. As a result, home ventilator patients do not always receive the full quantity of visits to which they are entitled. Says King, “I’ve got one patient who is allotted 20 hours of nursing care a week, but is lucky if a nurse is with him for even 10 of those hours.”
Compounding matters, the supplier of the home ventilator itself—the DME company—will not be reimbursed for sending a respiratory therapist out to the patient’s residence. Yet, the company must do precisely that in order to be accredited (something Medicare and other payors now require as a condition of doing business with them). King asserts that the problem of the nursing shortage and the need for DME companies to provide clinical support can be addressed in one fell swoop by assigning respiratory therapists to pick up the slack. “It would make good sense if payors were to reimburse for RTs to supplement the ranks of nurses and let us handle the ventilator-related issues in the home,” she says. “RTs are not as costly as nurses, would be perfectly appropriate and safe in this role, and could help take the quality of care in the home to the next level.”
Fighting the Good Fight
Still, the reality on the ground is that many payors likely will be unmoved by reasoned—and reasonable—proposals such as King’s. They will instead continue being miserly. They will pay a pittance for home ventilator equipment and support, and they will seek to forestall paying even those skimpy sums by employing a variety of tactics. Fortunately, there are ways to counter them, King assures.
“Adhering closely to insurer-supplied medical necessity guidelines is important, as is submitting proper documentation and, of course, obtaining preapproval prior to discharge,” she says. “If your claim is denied, you should appeal fearlessly because it’s usually worthwhile to fight. But a lot of people who receive a denial notification simply accept it. They don’t want to go through the process [of squaring off against the payor].”
As evidence that appeals work, King cites her experiences battling for a power-sharing system developed by Richardson Products. “It’s called the PTV, and it enables a portable ventilator to be powered by a wheelchair’s battery,” she says. “But because it’s a new product, payors often reject it out of hand”—as they did to one of King’s adult male wheelchair-using patients in Minnesota. “His ventilator battery often used up its charge while he was out and about in the wheelchair. Putting a PTV on his chair would have extended the run-time of his ventilator, giving him a greater measure of safety. The only other option would have been to add a second battery to the chair.” This was unfeasible, though: The addition of that second battery would have entailed modifications that would make the wheelchair too bulky to fit aboard public transportation. King emphasized that problem in her claim appeal. “I also presented very specific details about how PTV was necessary for the patient’s safety, not just his accessibility issues.” In the end, the payor relented and approved payment for the product. “The lesson is that you have to explain why the patient needs this particular piece of equipment or service. Beyond any issues of convenience, you have to be able to show specifically how having it will improve the outcome for this individual.”
Teach Them Well
Success in surmounting the obstacle of reimbursement can usually be extended to other home-ventilator challenges. Take the issue of information overload. One obvious remedy is thorough instruction of the family and friends to prepare them for their new and difficult role. “It is essential that those who will be caring for the patient receive proper training,” says Edwin Coombs, MA, RRT, senior marketing manager of respiratory care systems at Draeger Medical Inc, Telford, Pa. “Preferably, this training should take place in advance of the patient being discharged from the hospital. Proper care of the tracheostomy is essential, so family members must be properly trained in cleaning, suctioning, and maintaining the patient airway. Training on what to do during an emergency situation—and being prepared for those situations in advance—can make a tremendous difference in the outcome.”
Refresher training can take place during clinician visits to the home, Coombs suggests. “Gauge family and patient compliance with a particular treatment regimen and their understanding of the training that was presented when [the patient was] discharged from the hospital,” he says.
Training can be made more relevant if first an assessment of the home is made. Says King, “Look for signs of anything in the home that could create unsafe conditions for the vent patient,” such as the absence of a battery backup or an uninterruptible power supply (either being essential to keeping a ventilator in operation during an electrical blackout). Meanwhile, safety may be out the window if oxygen tanks awaiting use in conjunction with the ventilator are stored near an open flame or other dangerous location, she adds.
Subsequent visits to the home should include equipment inspections to make sure all is properly functioning. Also, a visit should be seen as an opportunity to check supply inventories and order more if quantities appear low. Clinical assessments can be part of the visit, if so ordered by the physician. “You would want to look at essentially everything that is looked at in a hospital setting: heart rate, breath sounds, peak flow, vital capacity measurements, airway patency, and anything else requested by the doctor,” says King. As to specifics, Coombs advises assessing the patient’s pulmonary status, vital signs, O2 saturation, and secretions. “Observe any changes in the ventilator settings or measured values that could indicate a change in patient condition,” he says. “During RN visits, medications and patient compliance should be monitored. Also, the dignity and independence of the patient are extremely important, so make sure proper mobility devices are available and proper support devices are installed.”
Coombs believes that home care RTs “must serve as the ventilator patient’s advocate during the initial assessment as well as at all follow-up visits.” King concurs and offers that respiratory therapists need to be in the habit of thinking one or two visits ahead. “Try to determine what the patient’s future needs will be, and prepare accordingly,” she says.
Naturally, home visits consume time. A typical visit can last 30 minutes for a simple assessment of equipment functioning and home safety, on up to 90 minutes if clinical assessments and interventions are added to the mix, King calculates. The frequency of visits usually decreases as the weeks and months roll by. “In the very beginning, we may be seeing the patient daily,” she says. “Then, it becomes twice a week, or maybe just once a week. Before long, the period between visits stretches out to once a month. For the most stable patients, you’re visiting once every other month.”
It is possible that the timing and scope of home visits will be different in the future, owing to the continued march of technologic progress.
“Imagine routine patient and ventilator checkups being done instantly through information technology,” Coombs ponders. “Information technology will also become a routine part of home care so that a patient’s ventilator data could be transmitted to a physician’s office, DME provider, or other practitioner who is engaged by the patient.”
|
Read more about home care reimbursement issues in RT’s archives. |
As to what King foresees, it is a future of more Web-based documentation. “Data will be delivered directly to our handheld terminals so we can know in advance of arriving at the patient’s home how many vent alarms occurred during a certain time frame, and what events triggered those alarms,” she says.
These and other advances will likely result in more mechanical ventilation provided in the home, she predicts. “Patients are best served by being at home,” King says, acknowledging that home is where the cardiopulmonary system is. “I think we can look forward to not only more vent patients at home but also, hopefully, more involvement by RTs in that setting.”
Rich Smith is a contributing writer to RT. For further information, contact [email protected].