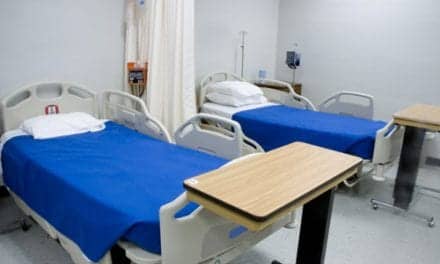
Mobile Medical Unit hallway with RT supplies on the left. Printed with permission of Mercy Health.
Life can change quickly. What is normal can be uprooted in seconds. Never was that more evident than the evening of May 22, 2011. At St. John’s Regional Medical Center, Joplin, Mo, the respiratory staff were making rounds in the intensive care units. The RT staff a few blocks away at Freeman Hospital were doing the same. Other therapists were sitting at home eating dinner or attending the local high school graduation, but at 5:30 that evening when tornado sirens sounded, life for Joplin RTs changed dramatically.
St. John’s Regional Medical Center
The RT staff at St. John’s found themselves in an unfamiliar setting that night. The hospital had taken a direct hit by an EF 5 tornado, which broke water, oxygen, suction, and power lines. Water was raining down from the ceiling, flooding the floors. Standing in the dark, staff used cell phones as flashlights to find crash carts, resuscitation bags, and oxygen tanks. There were more patients in need of ventilation than there were staff available to assist them, so environmental staff—and even visitors—were called upon to help with manual ventilation. Respiratory staff were able to ensure that all patients in need of ventilation that night were breathing. Oxygen tanks were rationed for the most critical patients. Other intubated patients were in need of endotracheal suctioning, so without suction pressure available, staff used 60 mL syringes with cut oxygen tubing to provide suction. Patients were carried down the stairs one by one and triaged outside. The sickest patients were placed in the back of pickup trucks and SUVs to be transported elsewhere for care. The roads were so flooded with downed power lines, trees, and building material that drivers had to forge their own paths to get patients immediately to Freeman Hospital. Meanwhile, those patients considered stable were held in a building with generator power about a block away on the hospital property. The patients were soon loaded into buses from three area school districts and shipped to hospitals around the region. Some traveled as far as 60 miles to find a hospital bed. By the time the night was over, 185 inpatients, 25 ED patients, and 270 staff had been evacuated from the hospital in approximately 90 minutes. There were many brave therapists working at St. John’s and Freeman when the tornado hit and others who immediately came to help. The names of these individuals can be found at the end of this article. Several therapists lost their homes and vehicles in the tornado, yet they continued to work and serve the community.
Freeman Health System

Across the street at Freeman Hospital, the respiratory department had had a slow day. After starting the day with six therapists, four were on staff at the time of the tornado, with 12 ventilators running in the critical care units. An emergency department physician who was resting in an off duty room recalls walking into the ED after hearing what he thought was a helicopter landing. He soon found out that what he had heard was not a helicopter at all—it was the tornado. He recalls the scene as a tsunami of injured patients. Every space in the ED was filled with patients covered in mud, insulation, grass, and blood. This mixture filled every orifice of the patients’ bodies. Six therapists scheduled for night shift quickly arrived to help with the chaos. The RT staff assisted the physicians as they treated many penetrating chest and head injuries. Ventilators were being set up so quickly that soon 24 were running. Having set up all available ventilators, BiPAP Visions (Philips Respironics) were cleaned and used as short-term vents. The recovery room was converted to an ICU, with many intubated patients being manually ventilated for extended periods by nurses, nurse techs, and even RTs from Mercy. Ventilators were brought to Freeman from Landmark, a nearby long-term acute care hospital. Freeman’s electronic medical record system was down due to limited power supply, so the respiratory staff had to revert to paper charting. Often before a chart could be completed, the patient was quickly stabilized and shipped to the nearest available critical care bed. By the end of the evening, 28 ventilators were running in Freeman’s CCU, but many more had been set up and shipped out throughout the day. Freeman therapists were not working alone. That evening, at least three therapists from neighboring states—Nebraska, Oklahoma, and Arkansas—arrived to help (personal communication from Mike McFall, BS, RRT, Freeman Health System).
St. John’s – Memorial Hall

St John’s Memorial Hall. Printed with permission of Mercy Health.
Since the night of the tornado, respiratory staff in Joplin have provided care in many unusual settings, including a civic center, university, mobile medical unit (MMU), and modular hospital. The remainder of this article will describe the care provided by respiratory staff working in these environments.
The tornado hit St. John’s Regional Medical Center at 5:41 pm. By approximately 7:15 pm, all patients, visitors, and staff had been evacuated from the building. With nearly 8,000 structures in Joplin destroyed by the tornado and many citizens injured, St. John’s physicians and staff needed a facility for immediate care. A small civic center, Memorial Hall, was an emergency shelter designated by the city of Joplin. It quickly turned into a hospital hours after the tornado hit. Gauze, gloves, sutures, and other medical supplies soon arrived. Therapists began inventorying intubation equipment, BiPAPs, ventilators, oxygen tanks, nebulizers, and other critical equipment. Here many patients received chest tubes, sutures, and nebulizers—and at least one patient was intubated. Memorial Hall was transformed into St. John’s Hospital for the week following the tornado until the hospital was moved into a mobile medical unit.

Mercy Hospital emergency department. Printed with permission of Mercy Health.
Missouri Southern State University
Located in North Joplin, Missouri Southern State University (MSSU) opened an 85,000-square-foot Health and Sciences Building in August 2010. All health profession programs are located in this state-of-the-art facility. It was built to function as a training hospital for the university students. The facility has a total of 29 hospital beds with medical air, gases, and suction. Following the tornado, the simulation center for interdisciplinary education was utilized as an ICU/CCU unit, and 1 hour after the tornado, the Health and Sciences Building opened its doors. Working with Joplin and Jasper County officials, the university designated the Leggett and Platt Athletic Center as a Red Cross shelter. Faculty and students from all the health profession programs at MSSU, together with more than 500 volunteers, provided medical services to 1,200 patients during the first week. The respiratory instructors, together with students, sorted medical supplies and provided oxygen therapy and nebulizer treatments. Respiratory staff at MSSU also worked closely with several local suppliers to help restore home medical equipment to patients who lost everything in the storm (personal communication from Tia Strait, Missouri Southern State University).
St. John’s – Mobile Medical Unit
Three days after the tornado decimated St. John’s, a Disaster Medical Assistance Team (DMAT) arrived on the hospital property to erect a mobile medical unit. These units have been used to provide medical care in many diverse settings, such as Afghanistan, Iraq, and Greensburg, Kan, following a similar EF 5 tornado in 2007. These medical tents are built to withstand 100 mph-plus winds, extreme temperatures, and several inches of snow. They can maintain room temperature in all weather extremes from -30° to 140°. The DMAT team, with the help of the Missouri National Guard, had the hospital fully constructed in just 3 days. By Saturday, May 28, staff began arriving at the mobile hospital for orientation and safety training. Before entering the facility, staff had to be trained on traffic flow, fire and weather safety, biohazard containment, isolation patients, and supplies. Without liquid oxygen, respiratory staff used oxygen concentrators to provide low flow oxygen and H tanks to provide high flow. An oxygen manifold system was constructed to provide oxygen from flowmeters as needed. Fuel generators provided electricity while also powering the air-conditioning system. The hospital was assisted with mobile trailers to provide two OR rooms, a cath lab, and imaging services. One week after the tornado, May 29, St. John’s opened the doors of the MMU at 7:00 am and received its first patient at 7:03 am. The first minor surgery was performed that same evening. With the opening, St. John’s Regional Medical Center’s name changed to St. John’s – Mercy Hospital. Respiratory staff worked in the MMU for 5 months until a modular, hard-sided structure replaced it in October 2011.

St. John’s – Modular Facility
St. John’s respiratory staff welcomed the modular hospital building. This portable building provided hard walls and a roof. Wall suction and oxygen were again restored to designated rooms. Electricity replaced the fuel generators, reducing the noise level around the hospital. Patients in the emergency department and medical units were provided more privacy with individual rooms. Respiratory once again had a department to call home even though it was small. The RT department was 96 square feet—8 x 12. The department could contain only one five-level shelf to hold respiratory equipment, and with limited inventory and the supply department located several miles away, hospital staff made deliveries every 2 hours to keep the hospital fully supplied. A few times a month, a therapist might make a run to the warehouse for items such as tracheostomy supplies, disposable resuscitation bags, and oxygen tanks. The RT staff found out how important organization is with limited floor space and have faced other challenges, such as quickly learning the nuances of new medical equipment. Mercy leadership decided to replace all the medical equipment associated with the tornado with new equipment. Often equipment is upgraded to newer models or replaced with another brand of equipment, and RTs have been involved in the decision-making about some of the items such as ventilators. Staff have learned to look at features that previously might have been overlooked, such as battery life.
There are many more stories respiratory therapists in this area could share. Facilities like Landmark Hospital, St. John’s – Mercy Hospital, Mercy Hospital – Rogers, Mercy Hospital – Springfield, Cox Health, Via Christi, Integris, McCune Brooks Hospital, and others received high patient volumes with the evacuation that night. Many therapists did not wait for the disaster call to come to work. They immediately put on their scrubs and drove to work upon hearing the news. Those who were not working in the hospital were in the Joplin area helping dig out friends and neighbors. So the list of names of therapists working that night is not exhaustive. It is merely a list of those working in Joplin hospitals when the tornado hit. This list is an attempt to honor them for their bravery that night. There were likely other therapists involved in Joplin that evening. On behalf of therapists everywhere—thank you to you all.
Christopher Cox, BS, RRT, is an education coordinator and American Heart Association Training Center coordinator for Mercy Hospital – Joplin, Joplin, Mo. Cox arrived on the tornado scene at 7:30 pm on May 22 and assisted with the transportation of patients off hospital property. Since the tornado, he has been involved with different types of education as staff move through the different hospital facilities. For further information, contact [email protected].
RT Staff Working at Joplin Hospitals May 22, 2011
St. John’s Hospital
Amber Crumbo, CRT
Teri Cuthbert, RRT
Debra Holmes, RRT
Sara Idleman, RT aide
Tom Ludwig, RRT
Donna Overton, RRT
Karen Sandberg, RRT
Rivian Vendetta, CRT
Jessica Webb, RRT
Kyle Willard, RRT
Jim Wray, CRT
Freeman Hospital
Misty Ray, CRT
Charlott Johnson, RRT
Traci Bowling, CRT
Alicia Theil, RRT-NPS
Chip Chesnut, RRT
Susan Stolte, RRT
Mary Jo Treiber, RRT
Jayma Lewis, RRT
Jeff Billingsley, RRT
Casey Schutterle, RRT
Tim Stark, RRT
Rachel Russell, RRT
MSSU Respiratory Instructors/Support Staff
Tia M. Strait, RDH, EdD.; Dean, School of Health Sciences, Public Safety and Technology
Glenda Pippin, BS, RRT-NPS, CPFT
Janice Dunaway, MS, RRT
Sherry Whiteman, BS, RRT
Caleb Lewis, BS, RRT