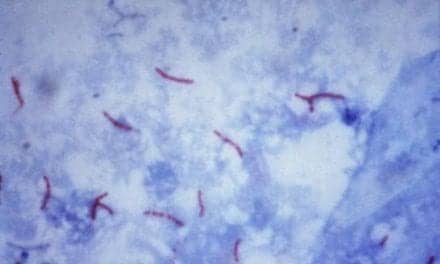
The etiology of sarcoidosis is unknown, but clinicians can treat the disease and improve the quality of life for those who suffer from it.

Sarcoidosis preferentially affects adults who are younger than 40 years of age. There seems to be a slightly higher incidence in females, and blacks appear to be affected more often than whites. Blacks from the United States seem to have the highest incidence of sarcoidosis in the world.2 Some scientists have suggested that the illness is far more severe in blacks and that whites are usually found to be asymptomatic.3 Approximately 30% to 60% of cases of sarcoidosis are discovered during screening chest radiography of patients who are otherwise asymptomatic, so the exact prevalence of the disorder is unknown.
Clinical Manifestations
Sarcoidosis involves the lungs in more than 90% of patients who develop the disease. The most common symptomatic complaints in these patients are dyspnea, chest pain, and dry cough. These symptoms are probably attributable to the presence of pulmonary lesions (frequently found in the alveolar septa and the bronchial walls) as well as to an inflammation of the interstitium and alveolar spaces that often precedes granuloma development.4 In rare cases, hemoptysis may be present. Five stages describing the extent of pulmonary involvement are used as reference points to classify disease progression (Table 1).5
| Table 1. Staging criteria for sarcoidosis. | |||
| Stage | Chest radiography | Additional findings | Regression |
| 0 | Normal | No abnormal findings | No abnormal findings |
| I | Bilateral hilar adenopathy | Enlarged lymph nodes | 75% experience spontaneous resolution within 1 to 3 years. |
| II | Bilateral hilar adenopathy; interstitial infiltrates | Enlarged lymph nodes; streaks in lungs | Two thirds of patients experience spontaneous resolution |
| III | Interstitial disease with shrinking hilar nodes | Interstitial opacities may be present in upper lung fields.Streaks in lungs; no enlarged lymph nodes | 10% to 20% experience spontaneous resolution |
| IV | Advanced fibrosis | Small lungs with streaks andspots; air cysts; peaks in diaphragm seen on x-ray. | None experience spontaneous resolution |
Most, if not all, cases of sarcoidosis involve more than one organ. In addition to the lungs, sarcoidosis occurs in the skin, eyes, lymph nodes, and liver. It may also affect the heart, nervous system, spleen, bones, joints, and various types of glands. Because patients are frequently asymptomatic, diagnosing the disease in all affected organs is extremely difficult; however, this is probably of little clinical significance in terms of therapy. Since up to one third, and perhaps more, of all cases of sarcoidosis involve the eyes, it is recommended that all patients being evaluated for this disease undergo eye examinations.6 Although most cases involving the eyes respond very well to treatment, in some cases, permanent eye damage may take place. In addition, up to as many as 35% of people who are afflicted with sarcoidosis develop skin lesions. These lesions frequently resolve without treatment.
Diagnosis and Treatment
For the most part, diagnosis is based on clinical findings and the results of radiographic examination. It is important to rule out infection from other causes. According to guidelines published by the American Thoracic Society,7 a comprehensive evaluation that includes history and physical examination, chest radiography, urinalysis, electrocardiography, an ophthalmologic examination, tuberculin skin testing, pulmonary function testing (with spirometry and diffusing capacity), and peripheral blood counts should be performed.
Corticosteroids are the most common treatment for sarcoidosis. In cases in which patients either do not respond to corticosteroids or cannot tolerate the treatment, alternatives such as the use of immunosuppressive, cytotoxic, and antimalarial drugs may be considered (although there is a lack of data regarding the benefits of these approaches to therapy).8 The results of a study9 examining patients who were refractory to conventional therapy suggested that treatment with anti-tumor necrosis factor will likely become the standard for treating such patients. Nonsteroidal anti-inflammatory drugs are often used to help reduce the inflammation associated with the disease, but not to treat the disease itself. Although the mortality rate of sarcoidosis is quite low, those patients who reach stage IV of the disease may be considered for lung transplantation. The risk of mortality is certainly increased in this patient population, although outcomes associated with lung transplantation in these patients are similar to those in patients who have undergone transplantation for other reasons. It has also been shown that race is an important factor that affects survival following lung transplantation.
Prognosis
The prognosis is typically good in sarcoidosis, although there are a number of conditions associated with poor prognostic indicators (Table 2). Prognoses for patients with stage-I disease are relatively good, while those of patients with later stages of disease are quite variable. All patients should be monitored at least annually, even if they are asymptomatic or have had spontaneous remissions. Follow-up visits should include physical examination, spirometry, and chest radiography. In the event that new symptoms are present during a follow-up examination, further studies may be indicated. Sarcoidosis patients who are experiencing significant respiratory symptoms may benefit from a course of pulmonary rehabilitation.
| Table 2. Negative prognostic indicators. |
|
Quality of Life
The most relevant or significant issue for the patient with sarcoidosis is probably that of quality of life. Although many patients experience spontaneous remission, 10% to 30% may continue to experience progression of the disease; this can affect both their ability to function and their psychological well-being.10 Clinicians are better able to understand a patient’s level of functioning if measures are taken to evaluate and document the quality of life from a patient-centered point of view. A cross-sectional study11 was recently performed to describe the health-related quality of life (HRQL) of patients with sarcoidosis. This study showed that there was a difference between the physician’s physical evaluation and the findings of a patient-centered HRQL survey. It is believed that HRQL measurements may provide a more useful assessment of the patient’s quality of life than traditional physiologic measurements. This study also found that patients being treated with oral corticosteroids showed a diminished quality of life. Increased levels of stress and depression among the patients evaluated in this study were also significant.12
Summary
Sarcoidosis continues to present the clinician with a challenging opportunity to treat a disease that is still relatively unknown, at least from an etiological and pathogenetic point of view. Continuing research will help to identify more accurately how to predict this disease, as well as its potential etiological factors.
Paul Nuccio, RRT, is director of respiratory care, Brigham and Women’s Hospital, Boston.
References
1. Thomas KW, Hunninghake GW. Sarcoidosis. JAMA. 2003;289(24):3300-3.
2. James GD. Sarcoidosis and Other Granulomatous Disorders. New York: Marcel Dekker; 1994.
3. Siltzbach LE, James DG, Neville E, et al. Course and prognosis of sarcoidosis around the world. Am J Med. 1974;57(6):847-52.
4. Takemura T, Hiraga Y, Oomichi M, et al. Ultrastructural features of alveolitis in sarcoidosis. Am J Respir Crit Care Med. 1995;152(1):360-6.
5. King TE. Overview of sarcoidosis. 2005. UpToDate Online 13.1. Available at: http://www.utdol.com/application/topic/print.asp?file=int_lung/ 2536&type=A&selectedTitl. Accessed May 21, 2005.
6. Newman LS, Rose CS, Maier LA. Sarcoidosis. N Engl J Med. 1997;336(17):1224-34.
7. Statement on sarcoidosis. Joint Statement of the American Thoracic Society (ATS), European Respiratory Society (ERS), World Association of Sarcoidosis and Other Granulomatous Disorders (WASOG) adopted by the ATS Board of Directors and by the ERS Executive Committee, February 1999. Am J Respir Crit Care Med. 1999;160(2):736-755. Review.
8. Baughman RP, Lower EE. Steroid-sparing alternative treatments for sarcoidosis. Clin Chest Med. 1997;18(4):853-64. Review.
9. Pritchard C, Nadarajah K. Tumour necrosis factor alpha inhibitor treatment for sarcoidosis refractory to conventional treatments: a report of five patients. Ann Rheum Dis. 2004;63(3):318-20.
10. Shorr AF, Helman DL, Davies DB, Nathan SD. Sarcoidosis, race, and short-term outcomes following lung transplantation. Chest. 2004;125(3):990-6.
11. Drent M, Wirnsberger RM, Breteler MH, Kock LM, de Vries J, Wouters EF. Quality of life and depressive symptoms in patients suffering from sarcoidosis. Sarcoidosis Vasc Diffuse Lung Dis. 1998;15(1):59-66.
12. Cox CE, Donohue JF, Brown CD, Kataria YP, Judson MA. Health-related quality of life of persons with sarcoidosis. Chest. 2004;125(3):997-1004.