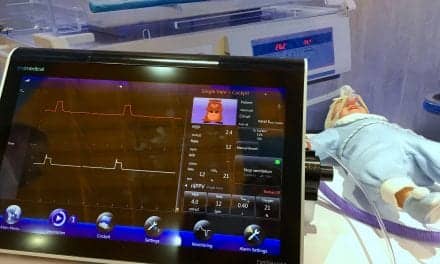
A video laryngoscope, due to its durability and portability, has proven to be a favored option for airway management during disaster situations.
By Phyllis Hanlon
In disaster situations, respiratory care practitioners have to think on their feet and act quickly. Take Hurricane Sandy for instance. When this “Superstorm” ravaged the New York/New Jersey coastline in 2012, hundreds of residents were displaced and many became ill, with a large percentage suffering respiratory difficulties from the toxic environment. Conditions such as shortness of breath, asthma attacks, and COPD exacerbated by anxiety and respiratory failure demanded immediate attention.
In cases like these, video laryngoscopy can effectively manage airways and facilitate better patient care.
A video laryngoscope, due to its durability and portability, has proven to be a favored option for disaster situations. Lightweight, waterproof, and battery-operated, the video laryngoscope is the suggested device for difficult airway management for portable storage units, according to the American Society of Anesthesiologists (ASA). In addition, the ASA’s 2013 Difficult Airway algorithm cites video laryngoscopy as a viable alternative to difficult intubation.
Video laryngoscopy is reported to produce larger and brighter resolution images, making it easier for the clinician to intubate patients. Moreover, the video version is said to exert less force and less trauma than direct laryngoscopy, which is vital when patients have already been subjected to a physically distressing situation.
And research backs up these claims.
- A 2009 study by Nakstad and Sandberg demonstrated the advantages of video laryngoscopy in airway management in simulated entrapped patients.1
- A second study, conducted by Sakles and colleagues and published in the December 2012 issue of the Annals of Emergency Medicine, found that emergency department intubations were more successful with video laryngoscopy than with direct laryngoscopy.2
- And a third study using simulated patients supported claims of a shorter learning curve and higher first attempt to intubate success rates; this study also reported a decrease in dental trauma using video laryngoscopy versus direct laryngoscopy.3
While emergency medical services in large part have adopted video laryngoscopy, the military also has employed the device in combat zones, such as Afghanistan and Iraq. Medics pointed out that typical injuries on the battlefield involved damage to the mouth, pharynx, or glottis.
The equipment needed to address these injuries must be dependable and easy to use. Military personnel reported that Verathon Medical’s GlideScope Ranger video laryngoscope successfully treated airway damage caused by improvised explosive devices (IEDs) and gunshot wounds, notably without the risk of cervical spine trauma.
Not only does video laryngoscopy quickly and accurately open an airway, but it also factors into the growing trend toward telemedicine. During the procedure, a small camera captures images of the internal structure and sends them to any device with a USB port, such as an iPhone or iPad, for immediate viewing on-site.
The device also can send the image to a central hub at a medical facility where a team of medical professionals can assess the situation and offer additional treatment guidance. Since video recordings are saved, this feature could be a valuable part of debriefing following a disaster. Clinicians have the ability to review treatment offered at the time of the situation and identify ways to improve technique or certain procedures.
Although direct laryngoscopy is still preferred in some instances, video laryngoscopy could become the new standard of care. RT
Phyllis Hanlon is a contributing writer for RT. For further information, contact [email protected].
References
1. Nakstad AR, Sandberg M. The GlideScope Ranger video laryngoscope can be useful in airway management of entrapped patients. Acta Anaesthesiol Scand. 2009;53(10):1257–61.
2. Sakles J, Mosler J, Chiu S, Cosentino M, Kalin L. A comparison of the C-MAC video laryngoscope to the Macintosh direct laryngoscope for intubation in the emergency department. Ann Emerg Med. 2012;60(6):739–48.
3. Rabiner J, Auerbach M, Avner JR, Daswani D, Khine H. Comparison of GlideScope videolaryngoscopy to direct laryngoscopy for intubation of a pediatric simulator by novice Physicians. Emerg Med Int. 2013;2013:407547.