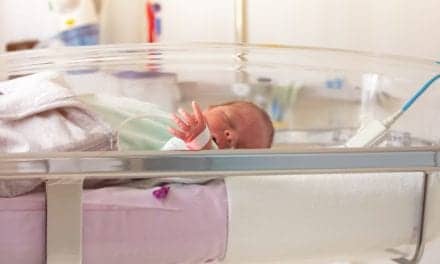
UC Davis’ respiratory care department has turned its attention away from day-to-day respiratory care; instead, it concentrates on critical care patients and consultation
In December 2005, the respiratory care department at the University of California Davis (UC Davis) Health System restructured in such a way that it now focuses most of its energy on critical care patients and is essentially a consulting service for medical floors. “Prior to restructuring our service model, we were a typical inpatient respiratory care department,” says Peggy Stulc, RRT-NPS, respiratory care manager for inpatient respiratory care at the hospital. “We now deploy our therapists to our 10 critical care units.” Stulc, who began working with the hospital in 2002 and was promoted to department head 2 years later, says that before the restructuring, therapists were stretched so thin that fatigue became a major issue.
The 565-bed teaching hospital typically runs at capacity and has undergone two major and a number of smaller expansions since UC Davis took title to the original facility, the Sacramento County Hospital, in 1973. Along with being an academic teaching hospital in the UC system, Davis is also the only level-one trauma referral site for the greater Sacramento area, and it is a tertiary referral center for surrounding states.
“The respiratory care department is a highly technical and specialized ancillary department that provides patient assessment and diagnostic and therapeutic procedures for adult, pediatric, and newborn patients with pulmonary and critical illness and trauma needs,” says Stulc. Before retooling its service model, Davis’ respiratory care department was short 14 full-time therapists. Thus, workload management and relief became top priorities. “We average 57 ventilator patients a day,” Stulc points out. “When we looked at our resources, we realized we needed to put our staff where the ventilators were.”

The department’s only full-time information technology specialist, Bob Hamilton, played a critical role in the restructuring process by upgrading the department’s computer program, Clinivision, to better reflect how the respiratory therapists were actually spending their time. “We had quite a few opportunities to improve the system,” Hamilton notes. “There were a lot of things that the therapists were doing on the floor or in the ICU that weren’t being captured.” For instance, he says, because nitrous oxide has both on-label and off-label uses, and the billing portion of the software program did not track administration of off-label treatments, “off-label use of nitrous oxide was falling through the cracks. So we created an off-label nitrous oxide order, which allowed the therapists to document their time.”
Prior to the restructuring, department therapists conducted an assessment on every patient who had respiratory therapy ordered and they administered the initial and all subsequent treatments. “We were understaffed. We had to restructure,” says the clinical coordinator for children’s services, Patricia Brown, RRT. Brown was also instrumental in designing and implementing the department’s current consult model, which redeploys the hospital’s respiratory therapists from floor duty to critical care duty, while creating a consulting function for medical floors.
“Now if a person with chronic obstructive pulmonary disease comes in for knee surgery, and a doctor writes an order to ‘continue at-home routine,’ ” she says, “we never see that patient unless the patient goes into distress.” The consult program has allowed the department to target patients most in need. For the new model to work, however, the department had to convince the physicians and nurses on medical floors that it was not abandoning those patients. “It took time for the doctors and nurses to buy into it,” says Brown.
One thing that really helped sell the new model was the “Rapid Respiratory Assessment Score,” a brief scoring tool developed by the department for bedside nurses on medical floors to use when uncertainty arises concerning the respiratory condition of a patient. If the score is greater than 10, the protocol is to ask for a respiratory consult. If the score is greater than 15, the nurse is instructed to call a physician. “It has put nurses at ease now that we aren’t on the floor all the time,” Brown adds. Stulc estimates that by shifting to a consult model, her department has reduced its workload by one nighttime and two daytime therapists. And because California mandates a nurse-to-patient ratio no greater than 1-to-4, nurses are able to handle the additional responsibility.
In recent years, the department also implemented evidence-based treatments. “The doctors, therapists, and nurses now all have more confidence in how we are treating patients, because it is all evidence based,” says Brown. Davis’ respiratory care department developed its evidence-based practice guidelines using those provided by American- and British-based thoracic societies and input from Davis physicians. Guidelines are based on a patient’s severity score and history. For example, Brown says, it used to be that a patient with pneumonia was automatically put on bronchodilators, but now evidence-based treatments have shown that only antibiotics, hydration, and nutrition are required for the treatment of community-acquired pneumonias, unless, of course, the patient is also an asthmatic. “By having an evidence-based program, we can concentrate our energy and resources on the people who need it most,” she says, because it helps to free up the therapists’ time.
Since the department restructured, the primary functions of the respiratory department in order of their priority now are: invasive ventilator management; trauma and emergency department response; management of specialty medical gases; attendance at high-risk newborn deliveries; resuscitation; internal transports; noninvasive ventilator management; pulmonary hygiene for patients in critical care units; medication administration for patients in critical care units; support of high-acuity patients outside critical care units; management of ventilator weaning strategies; assessment program for patient evaluation, consultation, and treatment plan; and arterial blood gas draws and interpretation.

Communication and skill competencies are also high priority areas for the department, yet in-person staff meetings proved nearly impossible because some employees, particularly those working part-time, can be off for several weeks running. “It was hard to get everyone in our department to come to meetings,” Hamilton says. “Communicating by e-mail didn’t work either. The therapists were reading their e-mails and then deleting them, so the information was lost. There was an information void.”
The department’s solution was to create an intranet. “Web sites are too static,” Hamilton notes. “So we created a Web application that allows people to update to it. Therapists can put up links to scientific data. We can post videos.” Hamilton recently posted a 2-minute video that walks the therapists through the computer application, and he says that vendors have already sent instructional CDs that detail the use of new equipment. Department therapists can watch equipment videos, take online continuing education courses, and complete some mandatory hospital and department competencies, either from home or from department computers during downtime. “Our system has a blog function, forum function, and wiki (open editing of Web pages) function,” Hamilton adds. “But it goes way beyond all of that.”
Staffing and Recruitment
The department currently has about 80 full-time respiratory therapists and another 20 or so work part-time. Two of Stulc’s full-time therapists report to the pulmonary diagnostic department conducting outpatient research in asthma management. All of the others work in the hospital. A clear hierarchy as well as a career ladder with five distinct levels helps Stulc’s therapists map out their career goals.
Excluding Stulc’s position, clinical coordinator is the highest rung of the ladder. “Clinical coordinators are registered respiratory therapists who assist the manager in overall clinical, financial, and performance improvement operations,” says Stulc. The clinical coordinator’s job is to assure that clinical and financial practices are followed as delineated by the department, the hospital, the university, and the state, and ensure that the mandates of all regulatory bodies, policies, standards, and legal codes are met. Clinical coordinators also direct the other four levels: RT I, RRT I, RRT II, and shift supervisor. Davis’ respiratory care department currently has two clinical coordinators: the education coordinator and the children’s services coordinator.
Four shift supervisors oversee the RT I, RRT I, and RRT II positions. “Shift supervisors are front-line representatives for the respiratory care management team,” says Stulc, and they assure by observation and audit that clinical and financial practices and resources meet all policy and procedural standards.
In concordance with the academic teaching duties and philosophy of the hospital, the department has an active teaching program that also acts as a recruitment tool.
“We provide clinical experience for three respiratory care programs, all of which offer associate’s degrees,” notes Stulc, whose department also extends externships to second-year students from the three affiliate programs. Externships are a good way for students to learn to care for hospital equipment and supplies at the same time they are learning about Davis’ respiratory care department. “Our goal is to introduce them to our professional culture, so they see us as an attractive place to work after graduation,” Stulc says. Two of Davis’ affiliate programs have proven to be good recruiting grounds; Five graduates from their spring classes are now employed in Stulc’s department.
The sheer size of the hospital and surrounding metropolitan area, along with the fact that Davis is an academic teaching facility, ensures a level of cutting-edge competency as well as a fluid, dynamic setting. Boredom does not even enter into the vocabulary of a Davis therapist.
Fran Howard is a contributing writer for RT.