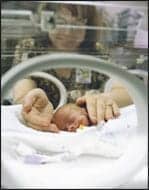
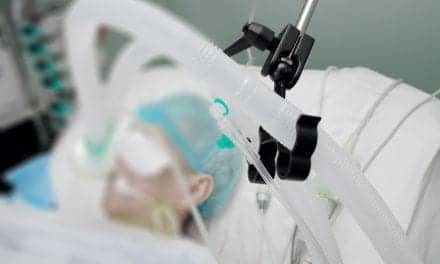
Successfully managing the nutrition of the critically ill patient necessitates performing a comprehensive and accurate assessment.

Enteral nutrition is the preferred route of nutrient administration in the critically ill patient. It maintains the integrity of the gut mucosa and has immunologic advantages over parenteral nutrition. Because it is usually not possible to start enteral nutrition immediately in the critically ill or injured patient, however, parenteral nutrition is an important therapeutic modality. Patients who cannot tolerate full enteral nutrition may be managed with parenteral nutrition alone or with combination feeding, a modality in which parenteral nutrition is gradually tapered off as the enteral formula’s use is advanced.
Generally speaking, calories and protein should be provided in amounts equivalent to energy expenditure so that a person can maintain nutritional status.1,2 In the critically ill or injured patient, energy expenditure may vary with the magnitude of the stress response.
Total Energy Expenditure
The rate at which the body uses energy (energy expenditure) is known as the metabolic rate. The basal metabolic rate or basal energy expenditure includes energy expended for such functions as breathing, circulation, and maintenance of body temperature. Normally, basal energy expenditure is measured in the morning, while the patient is still in bed. Resting energy expenditure (REE) is normally measured after a patient has rested in bed or reclined in a chair for at least 30 minutes, with no muscle activity and a thermally neutral environment. REE is about 10% greater than basal energy expenditure. The total of all the energy used by the body during all activities during the day is the total energy expenditure. Total energy expenditure includes basal energy expenditure plus excess metabolic demands.3

Differential oximetry is a relatively new technique. Arterial saturation is measured using a pulse oximeter. Mixed venous saturation is measured spectrophotometrically using a modified Swan-Ganz catheter containing a fiber-optic bundle. Cardiac output is determined using thermodilution. Differential oximetry is well suited to making frequent determinations of oxygen consumption.
The metabolic cart, a bedside metabolic analyzer of inspired and expired gas, measures oxygen consumption and carbon dioxide production. It is becoming the gold standard for nutritional assessment for critically ill and injured patients.
Subjective global assessment (SGA) is another method of rating nutritional status. SGA appears to demonstrate a good correlation between subjective and objective measurements.4 An SGA rating is obtained by using data from the patient’s history and physical examination, including weight change, dietary change, gastrointestinal symptoms, functional impairment, disease diagnosis, and physical findings consistent with malnutrition.4,5 Patients are rated as well nourished, moderately malnourished, or severely malnourished.

The fundamental goal of nutritional support for the critically ill or injured patient is to provide protein and calories in amounts sufficient to match the demands of hypermetabolism and increased protein breakdown. In addition, it is important to provide adequate micronutrients in order to meet the increased demand imposed by stress. Full nutritional support is generally not initiated immediately after injury. Reasons for the delay include the time required for accurate assessment, the need for resuscitation and/or early trauma care, and the potential complicating metabolic effects of aggressive feeding during the early, unstable period. Virtually all severely injured patients, therefore, experience a period of temporary starvation. Nutritional support should, however, be started as soon as possible after injury and should be maintained as long as the patient does not eat adequately.6 Support can almost always be initiated within 2 to 4 days after injury.
The current approach to the nutritional support of the critically ill or injured patient is to provide a broad array of the macronutrients and micronutrients that are necessary for health. If catabolic illness alters the requirements for specific nutrients, then the administration of required substrates might facilitate a patient’s anabolic response to a life-threatening illness.7 The route by which nutritional support is given may be an important determinant of outcomes.
Enteral Nutrition
If enteral feedings are possible, they are preferred, because enteral nutrition better maintains the integrity of the gut mucosa.6,8,9 Exclusive use of parenteral nutrition may be associated with a loss of the normal gut mucosal barrier, bacterial translocation, and (possibly) sepsis.6
Enteral nutrition should be initiated as early as possible, preferably within the first 24 hours after injury or intubation. Feeding a patient immediately after a severe injury or intubation can be difficult. The patient does not eat readily, may not be conscious, and may be dependent on ventilatory support. The route of administration depends on the patient’s condition and the type and severity of injury. Abdominal injuries may be associated with gastric stasis, in which case a catheter jejunostomy may be useful. With a catheter jejunostomy in place, a patient can receive enteral feedings only a few hours after an abdominal operation. Sufficient time is required to build up intestinal tolerance to enteral feedings. The concentration of solution is gradually increased; typically, feedings are initiated with 50%-strength isosmotic or hypertonic solution at 50 mL per hour. The solution is then changed to 75% strength and then to full strength. Next, the amount is increased to 70 mL per hour and, eventually, to 100 mL per hour.6 Full concentration can usually be achieved within 48 hours. If intolerance develops, it may take up to 5 days to reach the point of delivering sufficient calories to meet requirements.

The principal advantage of total parenteral nutrition (TPN) is that full nutritional requirements can be met within 12 to 24 hours. TPN is appropriate for patients who were malnourished before injury, are expected to have intolerance to enteral feedings, or need to return to the operating room frequently.6,8 A primary factor to consider when deciding whether to administer TPN is the functional status of the gastrointestinal tract.
TPN improves the nutritional status of most stressed patients.10,11 A mixed caloric regimen, relying on both glucose and fat as energy sources, appears to be best in the early postinjury period.12 This avoids exacerbation of hyperglycemia. A typical disadvantage of TPN is the possibility of intestinal atrophy. This atrophy may perpetuate multiple organ dysfunction syndrome.6 Definitive prospective, randomized trials are needed to clarify whether one route (enteral versus parenteral) has a distinct advantage over the other.
Peripheral Parenteral Nutrition
If only a short period of inadequate oral intake is anticipated and a central venous catheter is not desired (and can be avoided), the institution of peripheral parenteral nutrition (PPN) may be considered. The regimen is used for a few days, by which time most patients will be on full enteral nutrition or will be eating. PPN may also be considered for patients in whom early enteral feeding is contraindicated.
Combination Feeding
There is some evidence that points to the gastrointestinal tract as an important factor in the generation, maintenance, or amplification of catabolic responses to critical illness.13,14 Providing all or a portion of a patient’s nutrient requirements via the enteral route appears to be beneficial. When full enteral nutrition is not possible, nutrients can be provided by a combination of enteral and parenteral routes. Combination feeding is more physiologic than TPN alone.
During combination feeding, TPN can be tapered off when the patient is receiving more than 80% of his or her full protein and calorie needs enterally and is tolerating this well. It is important to check for clinical signs of gastrointestinal function before tapering off TPN. During combination feeding, it is important to monitor fluid status closely. It is also imperative to avoid overfeeding the patient, since providing nutrients in amounts greater than calculated or estimated needs may be more deleterious than starvation.
Summary
The stress response to injury, trauma, and/or disease is composed of characteristic and predictable biochemical and physiological processes: hypermetabolism, impaired protein synthesis, and catabolism, which lead to derangements in the metabolism of nutrients. The critically ill or injured patient requires appropriate nutritional repletion in order to reduce the loss of body protein and recover fully. Successful nutritional management for this patient population is predicated on performing a comprehensive, accurate nutritional assessment. The fundamental goals of nutritional support in this patient population are to meet the demands of hypermetabolism and increased protein breakdown.
Harold Rosenbloom, MD, is a contributing writer for RT Magazine.
References
1. Jeejeebhoy KN, Detsky AS, Baker JP. Assessment of nutritional status. JPEN J Parenter Enteral Nutr. 1990;14:S193-S196.
2. Roy LB, Edwards PA, Barr LH. The value of nutritional assessment in the surgical patient. JPEN J Parenter Enteral Nutr. 1985;9:170-172.
3. McCool C, Van Way CW III. Energy expenditure and its measurement. In: Van Way CW III, ed. Handbook of Surgical Nutrition. Philadelphia: JB Lippincott; 1992:119-131.
4. Eisenstein C, Van Way CW III. Nutritional assessment. In: Van Way CW III, ed. Handbook of Surgical Nutrition. Philadelphia: JB Lippincott; 1992:107-118.
5. Detsky AS, McLaughlin JR, Baker JP, et al. What is subjective global assessment of nutritional status? JPEN J Parenter Enteral Nutr. 1987;11:8-13.
6. Van Way CW III. Nutritional support in the injured patient. Surg Clin North Am. 1991;71:537-548.
7. Wilmore DW. Catabolic illness. Strategies for enhancing recovery. N Engl J Med. 1991;325:695-702.
8. Jones TN, Moore FA, Moore EE. Nutritional support following major trauma. In: Van Way CW III, ed. Handbook of Surgical Nutrition. Philadelphia: JB Lippincott; 1992:207-229.
9. Romito RA. Early administration of enteral nutrients in critically ill patients. AACN Clinical Issues. 1995;6:242-256.
10. Baker JP, Detsky AS, Stewart S, et al. Randomized trial of total parenteral nutrition in critically ill patients: metabolic effects of varying glucose-lipid ratios as the energy source. Gastroenterology. 1984;87:53-59.
11. Kafarentzos FE, Karavias DD, Karatzas TM, et al. Total parenteral nutrition in severe acute pancreatitis. J Am Coll Nutr. 1991;10:156-162.
12. Kudsk KA, Croce MA, Fabian TC, et al. Enteral vs parenteral feeding: effects on septic morbidity following blunt and penetrating abdominal trauma. Ann Surg. 1992;215:503-513.
13. Bessey PQ. Parenteral nutrition and trauma. In: Rombeau JL, Caldwell MD, eds. Clinical Nutrition: Parenteral Nutrition. Philadelphia: WB Saunders; 1993:538-565.
14. Wilmore DW, Smith RJ, O’Dwyer ST, et al. The gut: a central organ after surgical stress. Surgery. 1988;104:917-923.