A health services system in Nashville has merged its sleep centers to provide top-quality care and to ensure that its physicians remained
After weeks, even months, of staring at the clock every night at 3 AM, anyone would be at their wit’s end. That is why the Center for Sleep in Nashville, Tenn, treats sleep disorders, especially obstructive sleep apnea and insomnia, as if they were life-and-death emergencies. The center, of course, knows that sleep disorders are not true emergencies like heart attacks, strokes, or asthma attacks, but by the time the sleepless—or their bed partners—say “enough is enough,’ seeking treatment typically takes on a sense of urgency.
Two years ago, St Thomas Health Services decided to respond to that sense of urgency by merging its sleep centers and putting treatment for sleep disorders on a fast track. St Thomas Health Services, which had already been treating sleep disorders for a quarter of a century, also wanted to avoid market share losses due to the industry-wide trend of physicians leaving hospital-owned sleep centers to start their own. The resulting Center for Sleep has a business model that is a direct reflection of both goals.
-
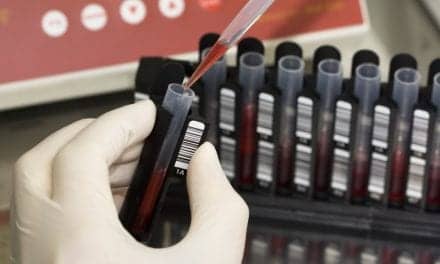
- From Left: Roger Pearsall, RPSGT – Staff Technolgist, Paul Anderson, RPSGT – Clinical Supervisor, Tabatha Burns, RPSGT – Staff technologist. They are reviewing a sleep study and discussing interscorer reliability.
St Thomas Health Services, which serves the Nashville metropolitan area, all of middle Tennessee, southwest Kentucky, and northern Alabama, consists of four hospitals: Baptist Hospital and St Thomas Hospital, both in Nashville; Middle Tennessee Medical Center in Murfreesboro, and Hickman Community Hospital in Centerville. St Thomas Health Services is owned by Ascension Health, the largest not-for-profit health system in the United States.
St Thomas closed the two small sleep centers in its two Nashville hospitals, St Thomas and Baptist, and opened its new center in an 8,000-square-foot, 14-bed remodeled facility, located across the street from Baptist Hospital. The newly merged Center for Sleep opened its doors for business on May 1, 2006. “The two hospitals had 12 beds. One hospital was running 6 nights a week, and one was running 3 nights a week,” says Edward Giannotti, Jr, administrator of the Center for Sleep. “Together, the hospitals were averaging eight to nine studies a night. Now we’re doing 11 to 12 a night. So we’ve had about a 20% increase in volume.”
Physician Investors
Keeping with its goal to prevent the defection of physicians from hospital sleep centers, St Thomas Health Services owns 75% of the center and six sleep physicians own the other 25%. The physician investors are medical director J. Brevard Haynes, MD; J. Michael Bolds, MD; Stephen Heyman, MD; Jon Tumen, MD; Bijoy John, MD; and Kirby Pate, MD.
This unique ownership structure of the for-profit Center for Sleep serves to provide a large referral network. “Our referral base is first and foremost our sleep physicians who are investors. Five are pulmonologists and one is a psychiatrist,” Giannotti notes. “From there, it expands to a peer-to-peer network of physicians who refer to the investors. Our referral base is quite large.”
The center’s reputation is based primarily on the reputation of its sleep physicians as well as the center’s technical staff, but its accommodations have also started to turn a few heads. “Our rooms have most of the accommodations of a high-quality hotel,” Giannotti says. While the accommodations are not quite five-star, he says, they are impressive, nonetheless. “We have Tempur-Pedic mattresses and pillows, cable TV, and private baths,” he adds. Patients typically check into the center between 7:30 and 8:30 PM. Before they check out, usually sometime between 6:00 and 8:00 AM, the center offers them a continental breakfast.
Patients have responded favorably. “They are taken aback by the accommodations,” says Gene Turney, RPSGT, CRT, community liaison for the center. Before leaving the center, patients receive a patient satisfaction questionnaire. Each question is graded on a scale of 1 to 4, with 1 being “poor” and 4 being “excellent.” Turney says that the center scores an average of 3.8 overall.
The center’s proximity to downtown Nashville is a real plus for the portion of its patients who typically commute 20 to 40 miles from the surrounding area to work in Nashville’s urban core. Approximately half of the center’s patient base is from Nashville and the surrounding metro area; the rest are from elsewhere in the St Thomas Health Services region.
Services and Staff
The center employees 14 technologists, all registered by the Board of Registered Polysomnographic Technologists (BRPT). Giannotti estimates that less than 60% of technologists in other sleep centers in his market are registered by the BRPT. “We have mandated that our technologists become registered sleep technologists,” Giannotti notes. “All of our technologists do the scoring and staging throughout the night,” which speeds up the diagnostic process and prevents treatment delays. Along with the BRPT designation, the Center for Sleep requires that all of its technologists be computer literate and competent in both file storage and data manipulation.
Three of the center’s sleep technologists also are either registered respiratory therapists or certified respiratory therapists, and one is a licensed practical nurse. All four technologists are dual-credentialed sleep technologists. “The Center for Sleep fully supports the BRPT as the gold standard for credentialing sleep technologists,” says Turney. “We oppose any movement by the American Association for Respiratory Care and the National Board for Respiratory Care to develop a separate sleep credential for respiratory therapists.” He adds that while the center recognizes the unique qualifications that a respiratory therapist brings to a sleep center or laboratory, respiratory therapists need to fulfill their polysomnographic technology education and become eligible for the BRPT examination before joining the staff.
The Center is staffed at a ratio of one technologist for every two patients. The center is open 5 days and 6 nights per week, and typically runs at about 85% capacity. “That’s basically full,” says Giannotti, because having a bed or two open to accommodate severe cases is preferable to running at 100% capacity. The center offers two nighttime diagnostic studies: polysomnography and polysomnography with continuous positive airway pressure (CPAP). It also offers two daytime studies: multiple sleep latency tests (MSLTs) and maintenance of wakefulness tests (MWTs).
Employees of the Center for Sleep are particularly proud of two homegrown programs. The first, called TEAMCARE, is a comprehensive oversight program for patients who require positive airway pressure therapy to treat their sleep-disordered breathing. “This is a focused disease-management program, much like the ones you would have for diabetes, heart failure, or COPD,” says Turney. “The obvious long-term goals are to assist patients in successfully self-managing their chronic conditions and minimizing morbidity and mortality.”
TEAMCARE involves the patient, the physician, the sleep center, and a home medical equipment provider, all focused on getting patients treated in a timely manner and preparing them to take ownership of the management of their disorder. To accomplish this, the center thoroughly educates patients on their disorders and lets them know what the risks are if they are left untreated. “Several of our sleep physicians do exits with patients the morning after the sleep study is completed,” and that is very unusual, notes Turney. This helps facilitate the fast-track treatment goal, which includes getting patients to the point where they are prepared to take charge of their treatment plan and getting them set up at home with any necessary equipment.
The Center for Sleep’s other program is called PROTECT. This program focuses on employees in safety-sensitive positions, such as truck drivers and health care workers. The center is currently working with the Tennessee Trucking Association to promote sleep apnea screenings for all commercial motor vehicle operators. It also offers free screenings for sleep disorders to employees in any of the health-services fields. “In light of [The Joint Commission’s] proposed 2008 National Patient Safety Goals, which include ‘prevent patient harm associated with healthcare worker fatigue,’ the Center for Sleep has developed a comprehensive fatigue management program,” Turney notes. The program consists of a sleep survey, screening for sleep disorders, and sleep education.
Big Investment in Technology
About one quarter of the total investment (between $1 million and $1.5 million) that went into developing the new sleep center was funneled into technology. This state-of-the-art sleep center has 22 PCs, one for each sleeping room, two in each consult room, and one for each person in management. What the center is most excited about, however, is its REMbrandt sleep system software (EMBLA, Denver), version 7.5, which provides acquisition and analysis of all sleep studies. Giannotti notes that in addition to what REMbrandt offers in terms of its technology, the software came with a one-time charge. That means updates are free as are ongoing maintenance fees.
“One of the neat things about REMbrandt is that all of the PCs that the doctors use [off-site] have the software,” notes clinical supervisor Paul Anderson, RPSGT. “REMbrandt says that putting copies on all of the doctors’ computers is okay.” This not only saves the affiliated doctors money, but it also allows them to read the results of the nighttime diagnostic tests first thing in the morning and develop a treatment plan, often even before the patient checks out. “As far as timeliness is concerned, we are number one,” Anderson notes.
The center also uses Respironics BiPAP Synchrony units primarily in the CPAP mode to treat sleep apnea. “They can also be used to treat other sleep-disordered breathing disorders such as central sleep apnea,” Anderson notes. A ResMed VPAP Adapt SV unit is used to treat central and complex sleep apnea.
The center also went entirely paperless earlier this year with the help of a new multiplex scanner that handles large batch jobs. “We put up to 50 documents on at a time,” says Anderson.
Technologists are currently involved with a clinical drug trial for the treatment of insomnia for a drug manufactured by Sanofi-Aventis. The center’s medical director is leading the trial, and the Center for Sleep is performing the protocol-required polysomnograms.
The Center for Sleep is a member of the American Academy of Sleep Medicine, the Tennessee Sleep Society, and the Natural Sleep Foundation. It also hosts interns from two nearby colleges, Volunteer State Community College and Columbia State Community College. Volunteer’s program is a 2-year sleep program, and Columbia trains respiratory therapists.
Sleep medicine is a highly competitive field, but the Center for Sleep has creatively found ways to best the competition. Perhaps most important, it has given sleep physicians an ownership stake, which prevents them from wanting to open their own sleep centers. Moreover, it has developed a fast-track treatment model that includes its physician investors, their referring doctors, and home medical equipment companies. It has also given patients a comfortable facility in which their condition is treated with the utmost professionalism and as if it were a life-and-death emergency because, frankly, that is often how it feels to the patient.
Fran Howard is a contributing writer for RT. For further information, contact [email protected].