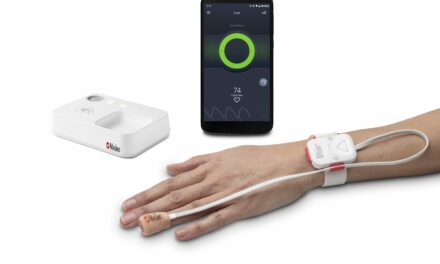
A focus on patient assessment and family education is important as RCPs continue to define their role in home care.

Home health care in the United States is a diverse, dynamic service industry. More than 20,000 providers deliver home health care services to approximately 8 million individuals who require such service because of acute illness, long-term health conditions, permanent disability, or terminal illness.1 Annual expenditures for home health care were $40 billion in 1997;1 the cost for coming years can only be imagined. The Health Care Financing Administration (HCFA) projects that the national expenditure for health care will total $1.15 trillion (1012) in 1998.
Over the past few years, growth in health care spending has slowed. Health spending grew at an average annual rate of 5.3%1 in 1997 and 1998, maintaining a slowed growth trend that began in 1996. In part, this slowdown in the rate of spending for health care has been attributable to the growing influence of managed care payment mechanisms and to the relatively low inflation rates seen for the US economy as a whole. For 2001 through 2007, HCFA projects an average annual growth rate for health spending of 7.5%.1
Since many out-of-pocket payments are made by home health care consumers to independent providers, and much additional funding for home health care is distributed to hospital-based agencies by payors other than Medicare and Medicaid, it is difficult to estimate home health care spending. The quality of respiratory home health care, however, has clearly become more important, since many hospital inpatients are now discharged earlier than they might have been in the past. An increase in the incidence of respiratory disorders has also been seen,2 along with increases in the amount and intensity of respiratory care needed by patients in the home. Chronic obstructive pulmonary disease (COPD), for example, is now the fourth most common cause of death in the United States. Its incidence has increased 41.5% since 1982, and there are more than 16 million US residents with COPD.2 The number affected by COPD could surpass 35 million by the end of this century. Mortality rates for cardiac and cardiovascular disease in the United States have decreased 45% to 58% since 1979, but COPD mortality has increased 32.9%.2
Home Health Care Services
Services provided in the hospital setting can nearly always be modified to suit the home health care setting. Many diagnostic, therapeutic, supportive, and life-support procedures can be performed in the home readily.
Patient assessment needs to be done on a continuous basis and with a high level of accuracy. Assessment must focus on the indications and contraindications for interventions, goal setting, the identification of higher-level services—such as psychosocial needs, invasive oxygen monitoring (ABG), and needs of physicians’ intervention—and frequent evaluation of the care plan. The evaluation of the patient’s respiratory condition during the assessment process will help RCPs to identify their roles in the care of individual patients and to determine the modalities needed to provide high-quality care in the home. An improperly trained RCP can administer prescribed treatment or therapy incorrectly and thereby hinder the patient’s safety.
Education
The RCP involved in educating home health care patients and their families can instruct them in infection-control techniques, in troubleshooting procedures that can be employed in the case of equipment malfunction, in the administration of therapy, in the modification of medication and supplies, in mechanical ventilation safety and the use of backup ventilation equipment, and in the procedures and protocols that should be applied in case of emergency. RCPS working in the home health care setting should familiarize themselves with specific modalities and procedures offered in the home.
Diagnostic Procedures
In the home, RCPs may be responsible for blood-gas sampling and analysis (home health care RCPs cannot qualify patients for supplemental oxygen therapy, however, as a conflict of interest could exist). They may also conduct pulmonary function studies (primarily spirometry), pulse oximetry and desaturation studies, the assessment of pulmonary mechanics (the determination of negative inspiratory force and minute ventilation), and, in some cases, the sleep studies needed to identify sleep apnea.
Aerosol Treatment
The proper use of metered-dose and dry-powder inhalers has been a problem for many patients; the RCP can correct many misunderstandings and promote the use of devices (such as spacers) that enhance drug delivery. There are so many devices available today that keeping up with aerosol-therapy technology can become a challenge. Multiple long-acting and short-acting b-agonists are available in inhaler form, along with several corticosteroids and other agents. The small-volume nebulizer is also used in the home; its maintenance needs are low, but patients need efficient instruction if they are to maintain its sterility and safe use. For tracheotomy and tracheostomy patients, continuous aerosol therapy powered by an air compressor may be provided.
Oxygen Therapy
Oxygen supplementation is the most commonly provided intervention in home respiratory care since the benefits of long-term oxygen therapy were established clearly in 1980 by a nocturnal oxygen therapy trial study group that documented the long-term survival of the COPD patient.3 Proper patient qualification is crucial to the provider’s ability to obtain reimbursement for such services. The type of oxygen-delivery device placed in the home by the home health agency depends on the patient’s needs and pattern of oxygen use. Physicians prescribing oxygen need to be familiar with what is best for the patients, bearing their individual circumstances in mind. Liquid oxygen systems are ideal for the active patient. Home oxygen concentrators are the most frequently used (and most economical) delivery system available. They are manufactured by several companies, and home RCPs should thoroughly understand each model now in use. Compressed gas cylinders may be too bulky for active patients, but are often used as a backup for oxygen concentrators in case of electrical failure in the home. When supplemental oxygen is used in the home, proper safety techniques are crucial elements in the RCP’s instructions to patients and their families.
Positive Airway Pressure Therapy
With the increasing incidence detection of sleep apnea and continuing improvement in sleep-diagnostic tools, continuous bilevel positive airway pressure devices in the home have become more common. These are available in a variety of types, but each calls for a great deal of instruction from the RCP. Proper instruction is likely to be the factor that will determine compliance and, as a result the achievement of the best patient outcomes.
Airway Management
Providing instruction in suction techniques and tracheotomy and tracheostomy care is clearly part of the RCP’s job in the home health care setting. Sterile techniques are taught to patients and their families, as are chest physiotherapy methods and the use of adjunctive equipment for the maintenance of good bronchopulmonary hygiene. Patients receiving transtracheal oxygen therapy delivery also need to be instructed in proper sterile techniques and maintenance to prevent infections and mucus plugging.
Supportive Therapy
Pulmonary rehabilitation techniques include breathing retraining, modifications that promote independence in the activities of daily living, physical reconditioning, inhaler use, and the application of coping mechanisms. Specialist RCPs from inpatient and outpatient facilities usually deliver these services. Because these are specialized areas, only a certain amount can be taught in the home. When patients do not have access to a rehabilitation facility, however, the home health care RCP plays a very important role in helping patients with COPD or asthma obtain a better quality of life.
With limited resources, an RCP in the home can also be very influential in helping patients find smoking-cessation techniques that fit their lifestyles. RCPs instructing patients in this area should receive additional training before they deliver smoking-cessation services.
Infection control is another important function; maintaining a sterile environment while using and cleaning respiratory equipment can be the key to successful recovery.
Monitoring and Life Support
Apnea monitoring for infants is commonly provided in the patient’s home. Background knowledge of pediatric respiratory care is necessary to the RCP’s proper delivery of instruction to the patient’s parents or caregivers.
The use of mechanical ventilation in the home has increased significantly over the past decade. Several factors have increased interest in home mechanical ventilation; among these are the development of compact, dependable, portable ventilators and the availability of trained RCPs. Both have helped payors decide that the home can be a less costly setting for mechanical ventilation. Thorough patient-selection processes and proper training of RCPs (and, in turn, patients’ families) are essential to the success of a home ventilator program. The home environment must be assessed and deemed appropriate and safe for home ventilation services. In addition, competent caregivers must be available.
Home Health Care Providers
The first home health care agencies were established in the 1880s. Their numbers grew to approximately 1,100 by 1963 and to more than 20,000 currently.1 Home health agencies, home aide organizations, home health care providers, and home hospice programs are known collectively as home health care organizations. Medicare’s enactment in 1965 greatly accelerated this industry’s growth. The number of agencies more than tripled between 1967 and 1985.1 The recent decline in the number of agencies is the direct result of changes in Medicare’s home health reimbursement, enacted as part of the Balanced Budget Act of 1997. The number of hospital-based and freestanding proprietary agencies has grown more quickly than that of any other type of certified agency since the coverage clarification. Freestanding proprietary agencies such as the Visiting Nurses Association now comprise 46% and hospital-based agencies 27% of all certified agencies. This differs markedly from the industry composition in the early 1980s when public health agencies dominated the ranks of certified agencies and proprietary and hospital-based agencies combined, accounted for only one-fourth the total.1 Traditionally, HME companies have employed the majority of RCPs in home health care, as these companies are the main providers of respiratory care in the home. Hospital and home health agencies also employ many RCPs.
The technology of home respiratory care also continues to evolve. Fingertip pulse oximeters and pocket spirometers can now provide accurate interpretations (and printouts) of test results; positive airway pressure devices have become smaller, less noisy, more convenient to use, more comfortable for patients, and more portable. Devices of all types are continuously becoming easier to use, for both patient and RCP.
In some areas, telemedical support is also available; homebound patients can be assessed and managed by a physician through video transmission accompanied by values for oxygen saturation, spirometry, electrocardiography, sleep data, lung sounds, and other physiologic data. This technology should not, however, replace the human contact so many RCPs deliver in the home.

References
1. National Association of Home Care Organizations. 1999 Home Care Statistics. Baltimore: HCFA; 1999.
2. American Thoracic Society. Standards for the diagnosis and care of patients with chronic obstructive pulmonary diseases. Am J Respir Crit Care Med. 1995;152:S77-S120.
3. Smith S, Freeland M, Heffer S, et al. The next ten years of health spending: what does the future hold? Health Affairs. 1998;17:5.