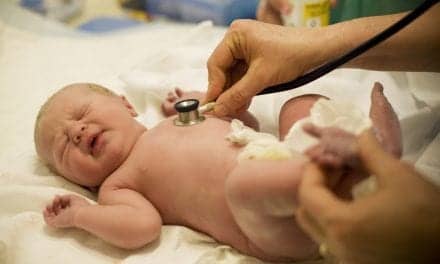
Classification systems: Similarities
There are two major systems or guidelines for asthma classification: One is from the National Asthma Education and Prevention Program (NAEPP) and the other is from the Global Initiative for Asthma (GINA).3 The NAEPP is affiliated with the National Heart, Lung, and Blood Institute (under the auspices of the National Institutes of Health) in the United States. GINA is a joint initiative between the National Heart, Lung, and Blood Institute and the World Health Organization. There are many similarities between the two guidelines (Table 1). Both have assessment and treatment based on age of the patient, with 5 years old being the division point. Both guidelines consider pulmonary function testing (PFT) or peak expiratory function (PEF) monitoring as feasible for patients older than 5 years of age.
Both the NAEPP and GINA guidelines use three areas to assess and score the patient: days with symptoms, nights with symptoms, and pulmonary function. Both use the same labeled steps to classify asthma based on these three areas. The steps are: mild intermittent (Step 1), mild persistent (Step 2), moderate persistent (Step 3), and severe persistent (Step 4). The criteria for pulmonary function are the same for both (they use either a comparison of measured FEV1 or PEF to the predicted value or a measurement of PEF variability.)

The list of symptoms is also the same for both NAEPP and GINA, and both state that the clinician should consider asthma if any of these symptoms are present. The list includes cough (with an emphasis on nighttime coughing), recurrent wheezing, recurrent difficulty breathing, and recurrent chest tightness. Both guidelines recommend assessing the patient to determine if symptoms occur or get worse at night and if symptoms occur and get worse when exposed to particular substances or situations (triggers). Both include the following as asthma triggers: exposure to animals with fur, airborne chemicals or dusts, exercise, viral infection, house dust mites, smoke (tobacco or wood), pollen, changes in weather (temperature), strong emotions (such as hard laughing or crying). Finally, both systems rely on the worst symptom to establish the level of severity.
Classification systems: Differences
There are some areas in which the two systems do not match exactly. GINA includes in the triggers two specific problematic drugs not mentioned in the NAEPP guidelines (aspirin, beta blockers). The NAEPP guidelines include mold and menses—not included in GINA—in the list of triggers. A minor difference is found in the wording: Times is used in GINA, whereas days (or nights) is used in the NAEPP. Two other differences are found when looking at the classifications within Step 1 and Step 2. If patients have <2 days per week with symptoms, the NAEPP classifies them as Step 1 mild intermittent, whereas the GINA guidelines specify <1 time a week to be classified as Step 1. The criteria for Step 2 include >2 days per week with symptoms (but not daily) in the NAEPP guidelines, whereas GINA states >1 time per week but <1 time per day for Step 2. One other significant difference is that the GINA guidelines for classification of severity take into account the treatment that the patient is currently receiving, so reclassification can be immediate after treatment begins. The NAEPP classification is designed to place the patient into one of the steps prior to initiation of therapy, and reclassification to a lower step calls for sustained control of asthma symptoms for at least 3 months.1,4
Problems in classification
Studies have looked at the application of these classification systems and have found that there are discrepancies and problems with trying to place patients into any one of the steps. In 2003, an article published in Chest5 examined the interrater reliability among pediatric asthma specialists using the NAEPP guidelines. Eight pediatric cases were presented in a survey sent to physicians practicing in several different states in the United States; 24 physicians received the survey, with 15 responding (one response was not sufficiently complete and not included in the results). Of the 14 physicians included in the study results, there were five allergists, seven pulmonologists, and two practicing in both allergy and pulmonology. These physicians categorized the cases using the NAEPP guidelines to designate the patient as Step 1-4 or “no asthma.” The cases gave such information as the patients’ medical and pulmonary histories, records of hospitalizations/ED visits, symptoms, lists of possible triggers, allergies, family histories, vital signs, physical examinations, chest x-ray results, PFT results, and reviews of their home environment for possible irritants. In the results, overall scoring described the interrater reliability as having poor agreement in classification of severity. The researchers noted that the clinicians had better agreement with each other in recommending a correct treatment regimen once the severity classification had been settled (for example, if the patient were considered to have moderate persistent asthma, the clinicians were in closer agreement in choice of treatment options).

In their concluding remarks, the authors noted that since the physicians received the same information, the differences and lack of agreement in asthma classification apparently occurred due to a difference in processing the information as opposed to the process of data gathering. They concluded: “Since some disagreement is clearly inevitable in the application of clinical judgment, the findings of this study should not be viewed as a criticism of pediatric allergists and pulmonologists but as a challenge to develop methods for reducing variability. As a first step, perhaps the expert panel of the National Institutes of Health, before releasing the next version of its asthma guidelines, should require a full-scale reliability study to ensure that the guidelines can be applied in a consistent manner by their intended users.”5
| Table 3 |
| NAEPP Guidelines: Four components of effective asthma management |
|
1. Measures of Assessment and Monitoring 2. Control Factors Contributing to Asthma Severity 3. Pharmacologic Therapy 4. Education for a Partnership in Asthma Care |
Another study published in 2005 in the Journal of Allergy and Clinical Immunology compared asthma severity classification by using the GINA guidelines, the NAEPP guidelines, and overall physician assessment in severe or difficult-to-treat asthma patients who were 6 years of age old or older but less than 55 years old (in order to reduce confusion related to the possible presence of COPD). Asthma symptoms were gathered using relevant questions from a patient questionnaire from The Epidemiology and Natural History of Asthma: Outcomes and Treatment Regimens (TENOR) study. Patients had PFT measurements performed at baseline. Enough data on 2,927 patients was sufficient to establish severity in the GINA and NAEPP systems and to determine that the subjects were the appropriate age. Overall, the study showed poor agreement between the three approaches in assessment of severity and placement into one of Steps 1-4. There was slightly better agreement between the physician assessment and GINA compared to the physician assessment and NAEPP. These results were thought to be related to the inclusion of medications in both the GINA and physician assessment processes. These authors concluded, “There is currently no gold standard for assessment of asthma severity.”4 Similar to the first study, the authors suggested that “improvement in the classification of asthma severity is warranted. Global asthma assessment should consider not only the patients’ physiologic and symptom measures but also recent medications and health care utilization.”4
Patient treatment
Once the classification has been established through either the GINA or the NAEPP assessment, treatment options follow. Both systems recommend providing the patient with a written action plan to explain what medications to use for usual asthma management and what to do if their asthma symptoms worsen. Both guidelines are very similar in recommendations for daily controller medications and treatment options (or alternative treatments) and education recommendations. As a result, the rest of this article will focus on the NAEPP guidelines to discuss treatment and education (Table 2).
Treatment for all patients diagnosed with asthma should include a quick-relief inhaled B2 agonist medication (frequently prescribed medications for quick relief include albuterol and levalbuterol). Sometimes the B2 agonists are prescribed in combination with the anticholinergic medication, ipratropium bromide. For patients classified at Steps 2-4, long-term controller medications are recommended. The preferred medication for this is an inhaled corticosteroid in a low, medium, or high dose—depending on the classification (Steps 2-4) and on the asthma symptoms. Fluticasone and budesonide are probably the most frequently prescribed inhaled corticosteroids. For Steps 3 and 4 (moderate to severe persistent asthma), the preferred treatment recommended by the NAEPP guidelines adds a long-acting B2 agonist to the inhaled corticosteroid therapy. The two medications recognized by the 2002 guidelines as long-acting B2 agonists are salmeterol and formoterol (both are available only as dry-powder inhalers or DPIs).
There are six goals of asthma therapy as mentioned by the NAEPP: minimal or no chronic day or night symptoms, prevent recurrent exacerbations and minimize emergency department visits or hospitalizations, no limitations on activities (no school/work missed), maintain (near) normal pulmonary function, provide optimal pharmacotherapy with minimal or no adverse side effects from medication, and meet patients’ and families’ expectations of and satisfaction with care. The guidelines state that one should step up to the next classification if control is not maintained. Once control has been maintained for 1 to 6 months, a gradual stepwise reduction may be considered.
Patient education
Patient education is considered very important to the success of asthma control. NAEPP guidelines designate education as one of the four components of effective asthma management (Table 3). Each visit to a clinic, office, and/or ED should include a thorough review of several topics and patients’ technique for administering their medications. Asthma patients have to be very involved in their self-management, and repeated education and instruction of these points help these patients remember what to do, how to do it, and when to do it. Unfortunately, time is often a limiting factor in the educational process, and this important aspect of self-management is sometimes sacrificed. Some facilities give the patient a brochure or handout that discusses asthma along with a written action plan that describes managing asthma in long-term control and what to do in case symptoms worsen. Table 2 shows the links between classification of severity and education. Each step includes six basic points that should be reviewed at every encounter; as severity increases, the educational topics also increase.
Another complicating factor in asthma management and patient education relates to the variety of delivery devices and equipment available for inhaled medications. Overall, there are approximately 20 medications available by metered dose inhaler; some contain a built-in spacer device. The inhalers include B2 agonists, corticosteroids, and anticholinergic medications. Optional spacer devices are available with built-in flow sensors, some have various masks to fit over the mouth and nose, others have a mouthpiece only, and still others are collapsible. Dry-powder inhalers have no propellant and rely on appropriate inspiratory flow to deliver the medication. In one DPI, the medication is packaged in the device and a counter tracks how many doses are left. Other DPIs require the patient to insert a capsule into a receptacle and puncture the capsule with built-in needles so the medication can be inhaled. Some medications are available only in unit dose and must be nebulized for delivery. Nebulizers use various aerosol generators such as a ultrasonic or air compressor to create the aerosol. Some nebulizers use a disposable handheld nebulizer circuit that connects to an air compressor by small-bore tubing—similar to those used in hospitals. Other nebulizers incorporate a “built-in” disposable nebulizer that is integral to the operation of the device.
Conclusion
Asthma is a chronic inflammatory disease with reversible airway obstruction—provided proper medication and disease management procedures are followed. Self-management is a major component of the approach to dealing with asthma. Education provides the foundation for proper medication administration, reinforces reduction of exposures to triggers, and motivates the patient to take steps to reduce or eliminate exacerbations. Classification of asthma severity is the starting point for deciding which medications to use and what components of education need to be covered. Although, as we have seen, there are problems in the classification process, the established classification systems (GINA and NAEPP) provide a framework for treatment and education, allowing for changes in patient condition, and give standards for performing research.
William C. Pruitt, MBA, RRT, CPFT, AE-C, is instructor, Department of Cardiorespiratory Care, University of South Alabama, Mobile.
References
1. National Asthma Education and Prevention Program. Expert Panel Report 2: Guidelines for the Diagnosis and Management of Asthma. Bethesda, Md: National Institutes of Health; July 1997. Publication No. 97-4051. Accessible at: www.nhlbi.nih.gov/guidelines/asthma/asthgdln.pdf Accessed March 3, 2006.
2. Sullivan SD, Weiss KB. The health economics of asthma and rhinitis. II. Assessing the value of interventions. J Allergy Clin Immunol. 2001;107(2):203-10.
3. The Global Initiative for Asthma (GINA). Accessible at: www.ginasthma.com/index.asp?l1=1&l2=0 Accessed March 3, 2006.
4. Miller MK, Johnson C, Miller DP, Deniz Y, Bleecker ER, Wenzel SE; TENOR Study Group. Severity assessment in asthma: an evolving concept. J Allergy Clin Immunol. 2005;116(5):990-5.
5. Baker KM, Brand DA, Hen J Jr. Classifying asthma: disagreement among specialists. Chest. 2003;124(6):2156-63.