According to investigators at The Ohio State University, new research in mice suggests an enzyme called Cbl-b may help maintain immune system function by ‘throwing away’ a specific protein that is typically responsible for controlling symptoms of allergic asthma.
The findings, published in Cell Reports, are the first to link Cbl-b to allergic asthma in an animal model, suggesting that the Cbl-b enzyme could be a target for drugs used to treat allergic asthma and other autoimmune disorders.
According to researchers, the findings parallel results from a 2012 Yale study in humans, which suggested that a mutation in the gene that produces Cbl-b was associated with higher risk for asthma in children. Other studies have suggested that inhibiting Cbl-b activity could reduce tumors and lower chances for cancer to spread.
Based on this assortment of findings, scientists believe Cbl-b could be manipulated in different ways depending on the disorder in question. Its activity could be elevated to keep excessive inflammation in check in people with allergic asthma, or it could be inhibited to treat cancer.
“We believe we have found one of the key molecules that can modulate the immune response,” said Jian Zhang, associate professor of microbial infection and immunity at Ohio State, and senior author of the study. “We can use this basic knowledge to try to find small molecules that can modify Cbl-b’s function and use this to treat human diseases that include autoimmunity, asthma and tumors.”
Allergic asthma is the most common form of asthma, and is triggered by inhaling allergens, such as dust mites, pet dander, pollen, or mold, leading to inflamed and swollen airways of the lungs, according to the American Academy of Allergy Asthma and Immunology.
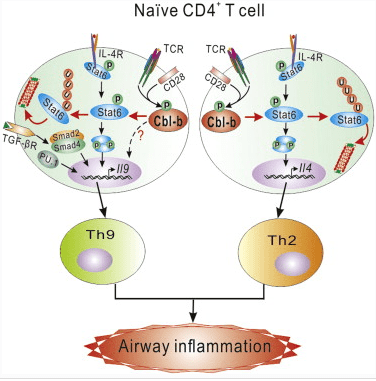
In this work, mice that are models for allergic asthma were injected with a substance that provoked an allergic response. Cells in the mice lacking the Cbl-b enzyme were unable to send a protein called Stat6 to a biological trash can once its services were no longer needed. With Stat6 active longer than necessary, two types of immune cells that it controls became overactive, eventually leading to excessive inflammation in the airways of these mice.
Mice with normal Cbl-b function had less severe allergic asthma symptoms.
Cbl-b is one of the key enzymes that participate in a process designed to keep protein levels stable in cells – in this case, cells that are present in the immune response. Cbl-b has the final step in the process, moving proteins whose job is finished to a space in the cell that functions as a garbage can, where they are degraded.
When the immune system is activated by a substance that generates an allergic response, cells called T cells are among the first responders. Once the invading substance is more clearly defined, a complex process transforms these general cells into different types of specialized T “helper” cells designed to fight specific invaders. Stat6 has a primary role in that T cell transformation.
Zhang and colleagues first determined in cell cultures that Cbl-b is needed in the general T cells to later control the activities of two types of T helper cells, called Th2 and Th9, involved in the allergic asthma response. But there is a step along the way that is critical to this process working properly: After Stat6 is activated by chemicals to help transform the T cells from general to specialized, Cbl-b must send the Stat6 protein to the garbage can.
If Stat6 is active for too long, it over stimulates Th2 and, to a lesser extent, Th9 cells so that they produce excessive inflammation in lung airways. Only Cbl-b can ensure that Stat6 doesn’t overstay its welcome.
The researchers further confirmed Cbl-b’s relationship to Stat6 in animal studies. In addition to observing that mice lacking Cbl-b became sicker than wild mice when exposed to allergens, Zhang deleted Stat6 from mice lacking Cbl-b to show that this protein, controlled by Cbl-b, was needed to push airway inflammation levels out of control.
“Without Stat6, Th2 was not active at all and Th9 was dramatically reduced. So we had minimal airway inflammation but not the abnormal, excessive inflammation present if Stat6 remains active,” Zhang said. “This suggests there is another factor involved in Th9. We don’t yet know what that factor is.”
Going forward, Zhang and colleagues will investigate Cbl-b’s potential role in the immune response to some infectious diseases. He notes his intentions to collaborate with pharmacy experts to develop small molecules that could modify the enzyme’s function.