|
Think caring for critically ill patients is difficult? Try doing it in a small, shaking box hundreds of feet above the earth.
“We try to replicate the ICU environment as best as we can in a small, cigar-shaped airplane,” says Francine Vogler, MD, medical director for AIRescue International, Van Nuys, Calif. Vogler, who helped start the company in 1992, adds, “Because the transfers we do are sometimes very complicated medical transports, ventilator demands are more complicated, so we need to have a respiratory therapist aboard.”
Breathing Easier
Whether the travel takes place in a fixed-wing aircraft, a helicopter, or an ambulance, RTs are—in ever-increasing numbers—joining the teams of medical professionals tasked with transporting the seriously ill.
Their inclusion in the field is a logical one: RTs are used to working in intensive care environments and bring with them a rich history of both medical training and assessment skills.
“Our strong background in anatomy, physiology, chemistry, physics, pharmacology, and microbiology makes us a big asset to the transport team,” says Dawn Filippa, RRT, EMT-P, a flight respiratory therapist with Hartford Hospital’s LIFE STAR, Hartford, Conn. “It used to be that respiratory therapists were only found in hospitals, but now a larger number are going to transfer programs, even when the patient is not being transported for respiratory issues.”
Although their primary role in most cases is to manage the patient’s airway, the very nature of a transportation environment often demands that RTs be adept at myriad skills. The assessment skills acquired through training and real-world experience are vital in on-site patient care.
“You are working with very little supervision, in a very dynamic environment, where you need to be able to think on your feet. If your equipment breaks, you’ve got to be able to make something work with the resources you have,” says Wes Ware, BS, RRT-NPS, EMT. Ware is a transport respiratory therapist for Angel One Transport, a program provided by Arkansas Children’s Hospital in Little Rock. “As less technology becomes available to you, the more you have to rely on your training in patient-assessment skills.”
As Part of the Ground Crew
Application of these skills is just as important for RTs who are not involved in traveling with patients, because they play a vital role in making the move a success. Properly preparing a patient before the transport team arrives will shorten time spent bedside, getting them on the road—or in the air—that much faster.
“There are a lot of things the RTs can do before we even get there,” says Ware. “They can obtain a detailed report of what treatments have been done and how the patient has responded to those treatments.”
Even seemingly minor, or routine, functions can save time and allow the patients to get to their destination faster. For example, if the patient is on a ventilator, the hospital-based therapists can order tests close to the scheduled move, so they are able to provide current laboratory values to the transport team.
“A recent ABG is helpful, because it tells us whether there are ventilation or oxygen issues. We need to know ‘What ventilator settings are they on?’ ‘What are the results of the chest x-ray?’ ” says Filippa, who also emphasizes the importance of properly placed ET tubes. If inserted either too far or not far enough, the tube must be reset and secured prior to leaving. “If the patient is intubated, they also should have an OG tube or an NG tube. RTs in the hospital aren’t trained to put those in, but if they can let the nurse or doctor know and get it put in, it helps save us time.”
 |
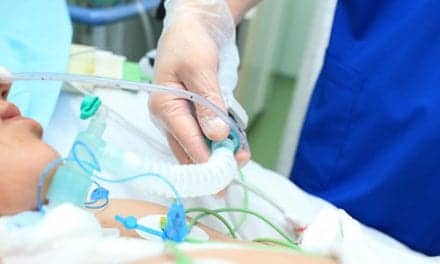
| AirRescue International’s Richard Hale, RRT, Tends to a tiny transport patient. |
Improving Care on the Run
While stationary facilities like hospitals and clinics have benefited greatly from health care’s rapidly improving technology, those who need these systems packaged “to go” have not always had the same luxuries. Before any piece of equipment can be introduced into the transportation environment, the team has to make sure it is a fit—literally.
“One of the challenges of this industry is finding equipment that does what we need it to do but is also portable and rugged enough for the environment that it’s going to be used in,” says Ware. Hours of constant vibration inside an ambulance, plane, or helicopter can shake a system into failure. “The first time we get a piece of equipment, the first questions we ask are ‘How much does it weigh?’ and ‘How far can we drop it and have it still work?’ “
Size also matters when it comes to machines intended for use by transportation teams.
“The smaller a piece of equipment is, the better it is for the transport environment. You can just imagine an ICU patient who is on a ventilator the size of a microwave or who is on a balloon pump the size of a washing machine, along with pumps and monitors,” says Vogler. “All of that equipment, and that patient, have to fit into an aircraft and be transported safely.”
Diminutive gear is also essential because often it must be carried by RTs when they arrive to retrieve the patient. Contained in handled bags, these packs include respiratory therapy equipment, intubation kits, a wide variety of endotracheal tubes, and other methods of ventilation. All of this is in addition to the standard intensive care supplies, such as medication, IV fluid, a portable pulse oximeter, C-collars, central line insertion kits, pediatric IV supplies, and all medications.
“On the actual gurney, we carry three big items: one is our oxygen caddy, which has our portable oxygen and all of the oxygen masks,” says Filippa, who is also the transport section chair for the American Association for Respiratory Care (AARC). “The other two are the end-tidal CO2 capnography machine and the big cardiac monitor.”
Inside the working space of the vehicle, RTs and their teammates have a wider range of equipment—in addition to ventilators—at their disposal.
“We have portable ICU monitors, which include ECG, blood pressure, and oxygen levels,” says Ware, who has more than a decade of experience in patient transport. His team also makes use of special IV pumps that are light and small and designed to remove excess air from IVs because, despite cabin pressurization, flying at altitude causes free air to expand. “We also have been carrying portable blood gas machines for about 10 years. We have really benefited from the ability to take 0.1 cc of blood and run it through our point-of-care testing machines to get pH, CO2, Po2, HCO3, BE, O2 saturation, sodium, potassium, ionized calcium, hematocrit, hemoglobin, and glucose.”
The helicopters used by Filippa and her colleagues are well stocked with a range of technology, including both noninvasive and invasive blood pressure monitoring, IV pumps and IV fluid warmers, pacers and a combined pacer/defibrillator, an onboard suction unit, a portable suction unit, and an intra-aortic balloon pump, as well as Doppler ultrasound.
“We can put in central lines in-flight and also have an Isolette with its own ventilator that we take for neonates,” adds Filippa. The team also carries more than 50 different types of medications: pain meds, sedatives, paralytics, thrombolytics, and all ACLS [advanced cardiac life support] medicines. “We have different types of rescue and surgical airway modalities, including Combitubes. We also can do pericardial centesis, needle decompression, and both pediatric and adult intraosseous insertions.”
AIRescue teams have access to a mobile laboratory, roughly the size of a brick, that allows them to perform blood gases.
“We recently got a stethoscope that connects to a monitor,” says Vogler. “It is the size of a laptop, and it can read cardiac function, as well as do modified ECGs.”
For Ware, who transports a large number of pediatric and neonatal patients, one of the most significant innovations has been the development of transport ventilators that make it possible to deliver nitric oxide in a mobile environment. Nitric oxide is delivered straight into the child’s lungs, to help alleviate pulmonary hypertension.
Evolving Essentials
In recent years, manufacturers have been meeting the demands of transport teams by packaging maximum performance into smaller packages. Perhaps the most vital advancement is the expanded functionality of the portable ventilators on the market.
“For us, the most important improvement has been to start to wean off the pneumatic ventilators to the ventilators that are compressor-driven,” says Vogler. These nonpneumatic machines help conserve oxygen. “We always calculate oxygen for the worst-case scenario, but you can never have enough. If you’re utilizing a ventilator that uses up all of your oxygen reserves and the patient deteriorates, then you can have a real problem.”
In general, ventilator technology has improved exponentially in recent years—much to the delight of RTs responsible for patient transportation.
“Not only has technology come along to where it can be downsized, but the battery technology has improved, so we can run [ventilators] for longer on battery power,” says Ware. New systems provide many different modes of ventilation and possess options similar to those available in larger versions, which provide additional benefits. “You want to switch as little equipment as possible between patients, so it’s vital that you can bring the same equipment and have it be able to ventilate all sizes of patients.”
Vogler’s teams often travel with patients on commercial airlines. These situations present a unique set of challenges. Oxygen must be ordered from the carrier—each of which has different requirements and stipulations of what can and can not be brought on board. Once on the plane, there are often other hurdles.
“You need to have the correct equipment, as well as the correct power requirements,” says Vogler. “Putting someone on bilevel, for example, draws much more electrical power than just being on a ventilator.”
The connectors on each airline are also different.
“With that kind of transport, it’s essential to have a respiratory therapist who is very experienced in air medical transport and in the transport environment,” says Vogler. “It’s not just a matter of intubating someone and bagging them, this is a little more complicated. It’s important to have someone who can problem solve, who understands if the connection is missing, and is able to come up with a way to make a proper connection.”
With their insatiable desire for smaller, more powerful systems, transportation professionals are always looking for the next “best” thing.
“Every year the technology gets better and better, but this is a field that is really ripe for invention,” says Vogler. “There are all kinds of things that can still be done, for example, how we can warm up the oxygen that we deliver into the patient, because there is no really effective way to do that in the aircraft.”
Regardless of how the technology advances, RTs are likely to be involved in putting it to use. Though the current industry standard is to employ nurses and paramedics who are cross-trained to perform ventilator management, those in the field are eager to see that shift.
“I would rather see more of the companies incorporate respiratory therapists on board the aircraft in the event of a transport, because they have more knowledge and more experience, and they can problem solve in the event of an issue,” says Vogler. “I believe RTs should assert their positions, because it is important and, certainly with the types of patients that we transport, they are invaluable. We wouldn’t want to transport without a respiratory therapist.”
Dana Hinesly is a contributing writer for RT. For further information, contact [email protected].