|
Once upon a time (say in the late 1980s), there was an anesthesiologist—or possibly two; there are different versions of events. This anesthesiologist—let’s call him David M. Gaba, MD, CHP/PCOR, fellow and professor of anesthesia and associate dean for immersive and simulation-based learning at the Center for Health Policy/Freeman Spogli Institute for International Studies and the Center for Primary Care and Outcomes Research at the Stanford School of Medicine in Stanford, Calif—was also a pilot.
Many hours of education and flight training are required for one to become a pilot. Unfortunately (or perhaps fortunately), pilots rarely have the opportunity to practice the aeronautical moves that could save their lives during an air emergency. So the industry developed flight simulators, in which pilots sit in lifelike cockpits and experience realistic weather and flight patterns. The simulator mimics real-life disasters so that the learning pilot can practice the proper moves and increase their chances of reacting correctly during a crisis. As a flight student, Gaba used these simulators.
Then, one day, perhaps while sitting in the simulator, it occurred to Gaba that the simulated flight situations reminded him of the events that occur in an operating room. “Dr Gaba recognized that the OR is very similar to the cockpit of a Boeing 747 in terms of the things that need to happen and the kind of breakdowns that occur in communication and situational awareness,” says Barry Grenier, BA, RRT-NPS, coordinator of learning and development in the respiratory care department of Children’s Hospital Boston.
The causes of jetliner crashes are not generally the pilots’ lack of skills, but the crews’ inability to act as teams in times of crisis. Medical teams can experience similar issues.
Realizing this, Gaba had a eureka moment and decided to bring simulation to medicine. Rather than “crew resource management,” he proposed “crisis resource management.”
“If you want to decrease the possibility of making bad decisions, everyone needs to practice, and they can do it in a simulator,” says Charles Pozner, MD, medical director of the STRATUS Center for Medical Simulation at Brigham and Women’s Hospital in Boston.
Over time, the medical community discovered that simulation is translatable to many different environments. Today, simulation has penetrated into nearly every area and discipline of medicine.
The Lessons
Simulation has been widely promoted among all phases of education, from community-based respiratory programs to bachelor’s and master’s programs to staff training. “Credentialing of practitioners using simulation is being discussed in many health care organizations, and maintenance of certification for some medical specialties is already in place,” says Thomas Belda, BA, RRT-NPS Technical Specialist, coordinator of simulation technical services, Mayo Clinic Multidisciplinary Simulation Center at the College of Medicine, Mayo Clinic, in Rochester, Minn.
The Mayo Clinic currently uses simulation to train allied health students, medical students, and resident physicians in many specialties, as well as nurses and other speciality medical staff. Orientation of new staff, evaluation of competency, as well as multidisciplinary training in the hospital setting, particularly in ICUs, are regularly performed. “The feedback we receive from participants in simulation education is that they really appreciate and often prefer this mechanism for learning,” says Belda.
Many facilities with simulation centers soon find they have too much demand. “Once people have begun to teach with simulation, they can’t get away from it,” says Pozner.
Simulation centers provide low-risk opportunities for learners to practice. Novice respiratory care therapists can become familiar with the setting, equipment, and processes of clinical care through realistic rehearsals of clinical situations. Participants get immediate feedback and can refine their techniques to deliver better care. Learners gain confidence and experience at all levels of care in an environment where the patient is not at risk.
Belda defines three categories of simulation: simulation using standardized patients or actors trained to play a role (in use for more than 30 years), mannequin-based training (the result of Gaba’s work), and virtual reality. “Computer-based simulation has been around for quite a long time, at least 20 years in respiratory care applications, but today’s training systems move closer and closer to the reality of actual surgical and emergency scenarios,” says Belda.
Lessons learned range from routine tasks to potentially rare experiences. Respiratory therapists can work on intubation, ventilation modes, and extracorporeal membrane oxygenation (ECMO), and they can practice with adult and pediatric mannequins.
At Children’s Hospital Boston, the ability to practice treating pediatric patients is a definite benefit. “You get better outcomes the more you perform something, so simulation provides the opportunity to practice [tasks and situations] not necessarily readily available. We’ll bring new grads into the simulation lab and let them practice basic airway management on a nonintubated pediatric patient, something they have probably not had to do in their training,” says Grenier.
Simulation can help respiratory therapists increase their value in the clinical environment. “If you are talking about volume and pressure [ventilation], you can put the simulated patient on a vent and say this is what the patient looks like on volume ventilation. Then you can switch to pressure ventilation, and students can see before their eyes what that looks like instead of having to wait and go to a clinical site and wait to see if a patient is put on a certain mode. So not only do they have a better understanding of what the two modes are like, but they know how they interact,” says Keith Hirst, BS, RRT, level II staff therapist at Children’s Hospital Boston.
Respiratory care therapists can also benefit on an enterprise level. In most simulation centers, respiratory care therapists are just members of one discipline that participates in multidisciplinary training, such as code teams, trauma teams, and surgical teams. At Mayo, respiratory therapists are a major part of the institution’s core group that provides educational and technical support as part of the operational staff within the center. Simulation is highly technical in nature, and respiratory therapists have many of the necessary skill sets to plug in and achieve highly successful simulation-based education programs.
“One of the problems historically with medical education is doctors trained with doctors, and nurses trained with nurses, and RTs with RTs. And when a patient got sick, they found they weren’t working with just their peers but as groups, so getting people to train in interdisciplinary settings is very helpful,” says Pozner.
The Twists
Of course, bringing everyone from multiple disciplines together to complete a simulated training program is not without challenges. Simulation centers require resources—and not just money. Space, time, and staff can be difficult to procure and retain. “Simulation programs are often started without the realistic accounting of time and staff necessary to guarantee their long-term success,” says Belda.
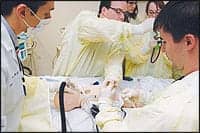
 |
| RT and nurse work together at Mayo Clinic’s simulation lab to suction a “newborn.” |
Many centers require a dedicated person whose time, whether part-time or full-time, is devoted to the center. “It really takes a dedicated staff person or people to keep a simulation facility going in terms of mannequin maintenance and the software updates,” says Grenier. This person may also champion the center, manage schedules, oversee curriculums, and teach; if not, the center may need employees who will.
“You need an expert who can get people through the daunting process of using simulation as a tool to teach,” says Pozner. A common mistake, according to Pozner, is thinking the simulation does the teaching, but the programs still require educators. The debriefing portion is key to the success of most simulation programs.
Debriefing requires audiovisual equipment, but simulated scenarios also require the simulated patient, the related medical technology, and the supporting equipment. “If you just have the simulator without the technology to intubate or insert an endotracheal tube, then that is a problem. You need to make it a useful, realistic situation,” says Pozner.
This, of course, requires money and space. “Simulation is indeed an expensive proposition, but deficits in training and education that lead to costly errors and mistakes with patients can also be very expensive propositions. Simulation factors directly as a necessary part in keeping quality high and reducing the numbers of errors encountered in the complex world of delivering health care today,” says Belda.
Pozner notes that institutions do not have to spend “millions and millions of dollars” on a simulation center. Smaller-scale models (eg, a room) may work as well. Hirst recalls that Children’s Hospital Boston started its simulation program in a space the equivalent of a closet (or thereabouts). “By the time you dragged in a vent and another dock and two other people, you were practically falling over each other trying to get in,” says Hirst.
Solutions exist: The important thing is to create a simulation program with the goals in mind. “If I were to develop a new center, the first things I would ask are who are we teaching, how are we going to teach, and how will we support it,” says Pozner.
Successful simulation centers will learn from themselves and others and continue to evolve over time. Since opening in 2005, Mayo Clinic’s has grown from a hospital-based program into a 10,000-square-foot dedicated facility on the edge of the institution’s downtown clinic campus. “Last year, we had just over 6,000 learner experiences in our center, and we are on pace to exceed that number this year,” says Belda.
A core group of faculty and staff regularly use the center to deliver curriculum to students in allied health and medical school programs, as well as graduate medical education for many residency programs including emergency medicine, pediatrics, anesthesiology, nursing, surgery, and respiratory care.
At Children’s Hospital Boston, the program has seen similar results in the 5 years since it has opened. “Our simulation program is becoming a victim of its own success. There is much more demand for simulation time now, and it is harder and harder to get time in the simulation lab for respiratory therapists,” says Grenier.
Not only can it be difficult to get time in a lab, but it can also be difficult to find time within the staff’s schedule, particularly staff on swing and night shifts. “We’ll take a therapist off nights and move them to days so they do simulated exercises,” says Hirst.
Schedules for multidisciplinary efforts can also be a struggle, with many scheduling factors that need to be considered. To make finding mutual time easier, Children’s Hospital Boston has its simulation program embedded in the medical surgical ICU. “This allows us at times to pull people from different assignments, cover them, and let them participate in some simulation activities,” says Grenier.
The program is also portable. The simulation program will go to the OR or the ER so the people being trained remain working in their own environment. “We are doing more and more of this,” says Grenier.
The Setting
Going into an actual environment increases the realism. “The simulation theater needs to closely represent the actual clinical environment in as many ways as possible, as this makes it easier for learners to ‘suspend their disbelief,’ ” says Belda.
Bringing in a multidisciplinary team can also get the heart racing. “I’ve been behind the curtain, but I can get into it and it becomes real. You feel your heart rate go up,” says Grenier. If the environment matches the objectives, the experience can become completely immersive.
“If you are trying to teach someone how to administer surfactant—as we do here because it is a low-volume, high-risk procedure—it’s important that our therapists can actually assess the patient, administer the surfactant using the equipment they would at the bedside…do an ongoing assessment, and respond to physiological changes,” says Grenier.
The environment for this learning experience will be different than that for a multidisciplinary team training on a cardiac arrest. The biggest limitations are the technology. “In aeronautics, you can simulate about 80% of a situation and lose about 20% of the reality. In medicine, it’s the opposite,” says Pozner.
Mannequins have come a long way however. In the middle of a recent simulation exercise, Hirst went to “pacify” the “baby” and stuck his finger in the mannequin’s mouth. “I realized the ‘baby’ was sucking on my finger,” says Hirst.
As technology continues to advance, the simulators will likely advance as well; eventually, patient mannequins will look as sick as they act. Costs will come down, and the number of tasks and procedures that can be run will increase. The resulting utility and return will continue to drive the expansion of simulation, not only throughout all levels of medical education but into new realms as well, such as research, product design, and process development. Gaba could not have imagined a happier ending.
Renee Diiulio is a contributing writer for RT. For further information, contact .