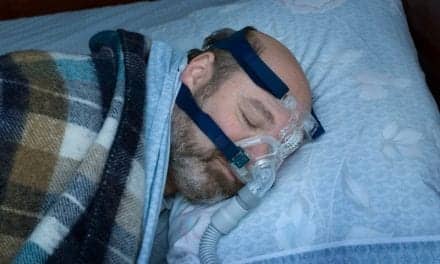
Clinicians who take pulse oximetry readings at face value do so at their own risk.

In the past decade since pulse oximetry has become as common at the bedside as thermometers and blood pressure cuffs, SpO2 measurements have been called the “fifth vital sign.” As a result, many clinicians take pulse oximetry readings at face value, which could be more dangerous than not monitoring SpO2 at all.
Potential Pitfalls in Pulse Oximetry
A recent article in the American Journal of Critical Care (AJCC)1 reported on a project in which clinicians’ baseline knowledge about pulse oximetry was assessed to determine if educational intervention was needed. A convenience sample of registered nurses, respiratory therapists, and physicians completed a survey composed of questions about pulse oximetry. Before completing an educational program, the percent of correct answers on the 17-question true/false survey was 76% for respiratory therapists (n=29), 66% for physicians (n=82), and 64% for registered nurses (n=331). To determine on which areas the educational intervention should focus, each question was categorized and analyzed.
At baseline, only 35% of nurses, 39% of physicians, and 76% of respiratory therapists knew that the statement “pulse oximetry is a method for continuous noninvasive measurement of arterial oxygenation and ventilation” was false. Forty percent of nurses, 35% of physicians, and 79% of respiratory therapists were aware that body position and ambient light can affect readings. And 39% of nurses, 46% of physicians, and 48% of respiratory therapists believed that “spot checks of pulse oximetry readings are as helpful in assessing a patient’s oxygenation status as the evaluation of continuous monitoring over time,” a statement not supported by the literature.
Areas in which baseline knowledge was high included knowing that significant hypoxemia is likely to occur during patient transport (96% correct), vasoconstriction and low pulse pressure can limit the ability to detect hypoxemia with pulse oximetry (95% correct), and patients are at increased risk for desaturation during invasive procedures (97% correct).
Several months after the educational program, the overall mean percentage of correct responses increased from 66% to 82% for all disciplines combined. While the clinicians’ knowledge improved, it would be interesting for this study to be replicated to see if increasing clinicians’ knowledge enhanced patient outcomes.
| More Pulse Oximetry Tips
• Probe placement on the earlobe is ideal for patients who have tremors or are shivering or restless. The earlobe is usually the only place you can get a reading during a seizure. • A pulse oximetry probe on the great toe can monitor perfusion of the foot following vascular surgery or injury to the leg that puts the patient at risk for impaired blood flow or compartment syndrome. Monitoring the plethysmograph output of the pulse oximeter will allow the clinician to see a change in arterial blood flow before it would be detectable by palpating pulses. • Do not use a pulse oximeter on a patient with suspected CO exposure. The pulse oximeter measures only the saturation of hemoglobin—the device cannot determine whether hemoglobin is saturated with CO or O2. • Know that patients’ hemoglobin levels will affect results. The fewer hemoglobin molecules present (anemia), the easier it is to saturate them. The SpO2 may be high, but total oxygen content will be low. On the other hand, if hemoglobin levels are high (polycythemia), it may be difficult to saturate the extra molecules with oxygen. This can result in major clinical workups to find the source of the so-called hypoxemia when the patient’s oxygen content may well be normal. |
Pulse Oximetry Perils for Patients and Clinicians
Anthony L. (Tony) DeWitt, RRT, JD, FAARC, an attorney with Bartimus, Frickelton, Robertson and Obetz in Jefferson City, Mo, and a practicing respiratory therapist for 13 years, emphasizes that pulse oximetry is only one monitoring tool, and the quickest way to wind up as a defendant in a malpractice lawsuit is to rely on pulse oximetry to the exclusion of other clinical assessment or monitoring data. DeWitt explains, “A pulse oximeter on the patient’s finger does not mean that the clinician is relieved of using his eyes, ears, brain, and clinical inquisitiveness.”
DeWitt describes a case from several years ago. “A man had an anterior approach for a C-5 discectomy, developed swelling, and required reintubation in the PACU (post-anesthesia care unit). Anesthesia orders said the patient should ‘remain intubated for 48 hours.’” However, the next morning, the medical doctor ordered immediate extubation, and the patient had stridor. “The medical records over the next 10 hours read like a textbook case of impending hypercarbic respiratory failure,” DeWitt says. “The patient became confused and combative, and with every combative episode, the nurses gave lorazepam or midazolam.” The patient ultimately arrested, and while the code was short and successful, the first arterial blood gas had a PaCO2 of 117 mmHg and a PaO2 of 45 mmHg. The patient suffered diffuse anoxic encephalopathy and was unable to return to work. “The nurses’ defense rested on their frequent charting of pulse oximeter values of 92% to 93%.”
Clearly, the nurses’ lack of understanding of the role pulse oximetry should play as one part of an entire patient assessment, and their reliance on pulse oximetry alone as the key factor in assessing the patient’s pulmonary status in this case were below an acceptable standard of care. However, the actions of these nurses are consistent with the findings in the project reported in the American Journal of Critical Care1 in which only 38% of clinicians knew that pulse oximetry did not provide any information about a patient’s ventilatory status.
Still, DeWitt would rather see a pulse oximeter used than abandoned. “In another case,” he explains, “a 42-year-old woman was breathless after a hernia repair. Her PaO2 on room air was 46 mmHg, and her PaCO2 was 29 mmHg. She was not transferred to intensive care, and no one even placed a pulse oximeter on her finger to monitor her hypoxemia. She ultimately expired as a result of anoxic encephalopathy, and the defendant pulmonologist testified he didn’t believe a pulse oximeter was necessary.”
The oxyhemoglobin dissociation curve illustrates the relationship between the partial pressure of oxygen dissolved in arterial blood and saturation. This physiologic phenomenon explains why an alarm set at 90% saturation may be too low for some patients and too high for others. The curve can “shift” to the right or to the left, depending on changes in arterial pH, temperature and 2,3 DPG (an organic phosphate that enhances the delivery of oxygen to the tissues).
Pulse Oximetry Pearls From the Bedside
Eileen Robinson, RN, MSN, a Pennsylvania nursing consultant, understands that not all clinicians learn a lot of technical information about pulse oximetry before they are asked to monitor patients with it. She has compiled tips that she reviews with nurses who will be using pulse oximetry. You may wish to share these key points with your nursing colleagues:
• Assess the site where the probe will be placed to make sure it is warm and has proximal pulses and brisk capillary refill. These quick assessments indicate perfusion to the probe site, which is critical for accuracy.
• Avoid sites distal to an automatic blood pressure cuff—when it inflates, blood flow to the sensor will be cut off, causing the pulse oximeter to alarm. This can decrease nurses’ vigilance if they automatically attribute an alarm to an inflated cuff.
• Check the patient’s temperature (and understand the relationship between the oxygen-hemoglobin bond and body temperature). If the patient is hypothermic, the bond will be tighter, meaning less efficient oxygen delivery at the tissue level. In these patients, you will want to maintain the SpO2 at a higher level than in patients who are febrile. When body temperature rises, the bond is loosened, meaning better oxygen delivery at the tissue level. These patients can usually tolerate a lower SpO2.
• Rotate probe sites as your facility protocol or manufacturer recommends. When placing the probe on the patient, be sure the photodetector and the light emitting diode are properly aligned.
Sarah Perry, RN, CCRN, MA, of Memorial Medical Center in Las Cruces, NM, echoes DeWitt’s concerns and confirms the results of the AJCC study.1 She says, “The common misconception is that if the SpO2 is good, then the patient is doing all right. Lots of nurses (and a few doctors) I’ve spoken with don’t give much thought to the fact that O2 saturation doesn’t tell us a thing about the patient’s CO2. Sometimes this results in a patient who is in big trouble while everyone focuses on the fact that the O2 saturation is just fine.” She also offers these tips:
• If your patient is on a cardiac monitor, compare the heart rate from the ECG with the pulse rate reported by the pulse oximeter. If the numbers are not consistent, you probably do not have adequate perfusion to the probe site.
• If the patient’s fingers and toes are cold and vasoconstricted, move the sensor to the earlobe for a more accurate reading. Remember not to turn the patient to the side on which the sensor is placed. It not only is uncomfortable but also can result in inaccurate readings.
You May Not Know…
Paul Mathews, PhD, RRT, FCCM, FCCP, FAARC, associate professor of respiratory care at the University of Kansas Medical Center, Kan, points out that many clinicians do not realize that SpO2 and SaO2 values are not equivalent. He says that some hemoglobinopathies can falsely elevate SpO2 if their light absorption pattern is similar to that for HbO2. Methemoglobinemia (Hbmet), sulfhemoglobinemia (HbS), and carboxyhemoglobinemia (HbCO) all will result in inaccurate results of both SpO2 and SaO2. In these cases, co-oximetry can differentiate types of hemoglobin in a blood sample.
Methemoglobinemia may be caused by a genetic deficiency in the enzyme cytochrome b5 reductase, and presents as cyanosis in an infant with no signs of hypoxia. It can also occur after exposure to chemicals such as nitrites and benzene and therapeutic agents such as nitric oxide, Lidocaine, and sodium nitroprusside (Nipride). Sulfhemoglobinemia has been associated with long-term use of metoclopramide2 and exposure to dimethyl sulfoxide (DMSO).
The widespread availability of pulse oximetry has been a major advance in monitoring patients with potential or actual oxygenation impairment. However, a SpO2 value cannot be taken at face value; it must be evaluated in the context of a complete patient assessment. Respiratory therapists can take the lead in replicating the AJCC1 study in their facilities, to identify knowledge needs across all clinical disciplines and provide education to enhance clinicians’ understanding of this important tool.
Patricia Carroll, RRT, RN,BC, CEN, MS, is the owner of Educational Medical Consultants in Meriden, Conn, and is the Health Care Coordinator for Shelter NOW, a homeless shelter in Meriden, Conn.
Reference
1. Attin M, Cardin S, Dee V, et al. An educational project to improve knowledge related to pulse oximetry. Am J Crit Care. 2002;11:529-534.
2. Aravindhan N, Chisholm DG: Sulfhemoglobinemia presenting as pulse oximetry desaturation. Anesthesiology. 2000;93(3):883-884.