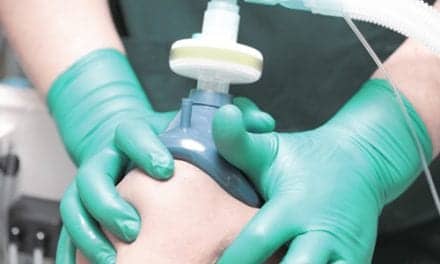
As hospitals press for high-quality, cost-efficient healthcare, respiratory care departments can add value to aerosol therapy in a number of ways.
By Mark Grzeskowiak, RCP, RRT, FAARC
When a respiratory care practitioner enters a hospital room, they bring with them their experiences, assessment skills, and the necessary equipment to the bedside in order to make a patient’s breathing a little easier. But in today’s healthcare environment, there is an increasing emphasis on becoming more productive. RCPs must be able to do more in less time and with fewer resources. This scenario can sometimes leave the RCP wondering which goal is more important: providing quality care, or completing more billable procedures.
In the case of aerosol therapy, value can be added to the treatment by increasing quality while decreasing costs. However, inexpensive products do not always provide a reasonable quality of care, and it is up to respiratory care departments to resist cost-cutting strategies that look good on paper but may compromise patient care. This article will focus on strategies that can allow RCPs to provide high-quality care and still keep budget offices happy.
Defining Value
The term “value” can be found in almost every product advertisement. It is applied to packages of frozen vegetables, it is incorporated into the name of hardware stores, and it is used to define fast food meals. Because it is used so commonly, it is hard to know exactly what “value” really represents. Value can be defined in more objective terms by the following formula:
Applying this concept to a respiratory care scenario, the value of a breathing treatment would be high if it was high in quality (relieved shortness of breath) but low in terms of the costs needed to provide it.
In terms of aerosol delivery specifically, other measures could be used to define the quality of treatment, such as:
- Particle size of the aerosol produced;
- Time required to deliver a nominal dose; and
- Amount of aerosol actually inhaled.
The cost of providing the treatment also determines its value. Factors that influence cost include:
- Acquisition of drugs and supplies;
- Ongoing maintenance;
- Costs for educating staff and patients; and
- Providing therapy of low therapeutic value.
For aerosol therapy, adding value can be accomplished in a number of ways: including the use of new equipment, applying new ideas to improve delivery of procedures, and better identification of patients who will and won’t benefit from the therapy. Examples of these will be discussed in this article.
Providing low value aerosol therapy could have drawbacks in a number of circumstances. Patients who receive inferior quality therapy in the emergency department are not only likely to spend more time waiting, they are also more likely to be admitted rather than discharged home. For admitted patients with chronic lung disease, low value therapy leads to increased length of stay. Meanwhile, patients who receive low value aerosol therapy at home using compressors or nebulizers are more likely to be readmitted if their equipment cannot provide them with relief.
Overall, delivering drugs in aerosol form has a number of advantages, but it also has been described as a relatively inefficient method compared to other medication delivery systems. For example, patients who receive drugs intravenously or in pill form receive a far greater percentage of the medication than patients receiving drugs via inhalation therapy. According to the AARC’s Guide to Aerosol Drug Delivery, a patient would normally receive only about 12% of the medication placed in the typical small volume nebulizer.1 Chart 1 illustrates why the percentage is so small.
Some of the medication placed in the nebulizer evaporates as it is being aerosolized. An additional amount will be aerosolized but will never leave the nebulizer—these are the droplets that form on the inside of the nebulizer and are referred to as the “dead volume.” Also, the patient will never receive any aerosol that is being produced while they are exhaling.
Adding Value with Equipment
One way to improve the value of aerosol therapy would be to improve the efficiency of this process. Nebulizers that incorporate the use of some type of reservoir have been shown to be helpful in this regard. One bench study that involved the use of isotopes and a variety of breathing patterns showed that a nebulizer with a reservoir had significant advantages over a breath-actuated type.2 The nebulizer with the reservoir delivered an equal or greater amount of inhaled mass in 4 minutes while the breath-actuated type took about 8 minutes.2 The differences in inhaled mass were more pronounced when a pediatric breathing pattern was used. The improved aerosol delivery efficiency allows for treatments to be shortened by 2 to 4 minutes. Particle size was not measured in this study, but previously performed independent studies report the particle sizes of the two nebulizers as nearly identical. The mass median airway diameter (MMAD) is 2.7 for the reservoir type and 2.8 for the breath-actuated type.
Cost is a factor that is frequently considered when new supplies or equipment is being purchased. It is important to realize that there are more components to the true cost of an item than just the purchase of materials. Items that need frequent servicing or repair or those that are difficult to assemble and require extensive staff or patient training have hidden costs that should be accounted for.
In the nebulizer study described above, the breath-actuated nebulizer was actually less expensive than the reservoir type, but a detailed analysis showed that purchasing the breath-actuated nebulizer would not translate into a savings for the medical center. This is because the device would not reduce the amount of time that a respiratory care practitioner would spend in the patient’s room.3 Using the more efficient nebulizer, the reservoir type, would allow for more time to be spent assessing and educating the patient, and this could be considered a value-added intervention.
The use of reservoirs has been a point of concern for some practitioners. They point out that the reservoir retains some droplets, and moisture in an enclosed space could be the perfect environment for bacterial colonization.

Figure 1. Condensation forms inside the reservoir but no organism growth was cultured in 252 samples.4
A recently published bench test of one reservoir nebulizer showed that this is unlikely to occur.4 Daily cultures of 53 patient nebulizers were performed. Twenty of these patients used their nebulizers for four consecutive days. After the patients took their treatments, the nebulizers were shaken out over a sink and stored in a plastic bag at the patient’s bedside. A total of 252 cultures were taken and no significant bacterial growth was reported.4 (See Figure 1.)
Vibrating mesh nebulizers were introduced in 2005 and may be another way to add value to aerosol therapy. In these devices, aerosol is produced when electricity is applied to a disc that vibrates at over 120,000 times per second. These vibrations draw liquid up through a series of over 1,000 holes that are drilled into the disc and produce a very fine, very dense aerosol. The diameter of the hole regulates the particle size.
Vibrating mesh nebulizers produce aerosol very quickly and have virtually no dead volume. Also, since they use electricity to produce aerosol, they do not influence the volumes, pressures, or oxygen percentages being delivered to ventilator patients. They have been shown to produce two to four times more aerosol than a conventional jet type nebulizer.5 Anecdotal reports indicate that patients receiving continuous beta-agonist delivered by vibrating mesh need the therapy for far less time than others who are receiving the same therapy delivered by a conventional large-volume nebulizer.
Adding Value by Subtracting
Another way to add value would be to eliminate aerosol therapy treatment for patients where there is no perceivable benefit. A scoring system has been developed by a Vermont hospital in order to assist its staff with focusing their efforts on the pediatric patients with the greatest need. The system is outlined in Chart 2.
By adding the scores for each category—breath sounds, response, pulse, respiratory rate (RR), and shortness of breath—a total “point value” can be determined to prioritize treatment.
- A total point value of 0-4 ? PRN.
- A total point value of 5-7 ? QID.
- A total point value of 8-10 ? Q4/PRN.
- A total point value of 11-12 ? Q2.
Bronchodilator therapy is commonly administered to patients requiring mechanical ventilator support, but the benefits are questionable when there is no bronchospasm and there are no observable improvements.

Figure 2 and Figure 3 represent pre- and post-continuous albuterol delivered by vibrating mesh nebulizer in a 34-year-old asthmatic. Note the difference in airway resistance (R) and peak airway pressure (Ppeak).
Where is the value in delivering beta agonists to patients in septic shock, or those with intracranial bleed? RCPs should be using ventilator graphics, pressure measurements, and their assessment skills to evaluate the effects of this therapy on their patients. If there are no significant changes in airway resistance, peak pressure, or ventilator graphics, there needs to be a discussion with the ordering physician about what the therapeutic objectives are. Figures 2 and 3 are examples of the response observed in an asthmatic patient who clearly benefited from bronchodilator administration.
Meanwhile, treating an infant or resistant pediatric patient with aerosol therapy can be challenging. Few of these patients will accept a mouthpiece treatment and fewer still will tolerate a mask. The alternative is to hold the nebulizer several inches from the baby’s face and to hope he inhales enough aerosol to produce a favorable effect. This is clearly an inefficient method.
In his editorial, “Bye-bye, blow-by,” Rubin points out that 40% to 85% of a loading dose is lost when a mask is 2 cm from a patient’s face.6 Many aerosol delivery studies on pediatric patients are performed using a manikin, so the amount of aerosol actually inhaled is questionable at best.
Aerosol delivery via a nasal cannula is perhaps a more viable option; however, one study using this method demonstrated that only 8% to 18% of a loading dose could be delivered through a system using nasal prongs.7 When considering a nasal cannula, it should be noted that the nose functions primarily as a filter—and not as an absorber—of medications.
Adding Value Through Change in Practice
Purchasing new equipment can be difficult to justify when administrators are looking for ways to reduce operating expenses but adding value does not always require spending more money. Delivery can be improved by changing the position of the delivery device in the circuit of ventilated patients.
An aerosol mask is sometimes the only interface that can be used to deliver a treatment. However, respiratory care practitioners must remember that drug delivery by mask can result in as much as a 50% reduction in the amount of aerosol delivered, when compared to a mouthpiece treatment. When the patient is unable to cooperate or seal their lips, a mask may be the only option.
But when a patient asks for a mask so they can continue a phone conversation or use their hands to play cards, this represents a compromise to their care. Aerosol therapy is not a very efficient way to deliver a drug, so why compromise the process even further by using a mask?
In their article on nebulizer placement, Ari et al showed that aerosol delivery varies significantly based on the device and its position in a ventilator circuit.5 Metered dose inhalers delivered more drug when placed between the wye connector and the patient. Conversely, jet nebulizers could be more effective if placed farther away from the patient. Placing the jet nebulizer on the dry side of the humidifier also may minimize the chances for bacterial colonization.
As Chart 3 illustrates, nebulizers were placed at two locations in the circuits of patients on continuous mechanical ventilation.5
The nebulizers in the top group were placed at the proximal airway. The nebulizers in the lower group were placed on the dry side of the humidifier. Each column represents 1 day. If a patient’s nebulizer was not available for sampling (patient expired, therapy discontinued, nebulizer changed out), the letters “N/A” appear in the cell.
Based on the results, within 48 hours some bacterial growth was found in all nebulizers placed at the proximal airway (top group). On the contrary, the nebulizers placed on the dry side of the humidifier remained organism free.5
Patients with a tracheostomy frequently receive aerosol therapy, and the way the nebulizer attaches to the patient can have a profound effect on the amount of drug delivered. The connections of many devices are of a common size and are easily adapted. But in some cases this may compromise the patient’s therapy. A conventional nebulizer can fit perfectly into the adapter on the trach collar, but how much medication does the patient actually get? Studies show that this probably is the least effective way to deliver aerosol to the patient.8
Work published by Ari et al shows that far more drug can be delivered to a trach patient if a resuscitation bag is attached to the circuit and manual breaths are used to deliver the medications.8 Chart 4 reveals that less than 7% percent of a loading dose was delivered to the lower airways of their study manikin using only a trach collar. By comparison, nearly 46% was delivered if a manual resuscitator was used to assist the simulated patient during inspiratory efforts.8 Significant improvements also were obtained when the artificial airway was an endotracheal tube.
Trust but Verify
The American public first heard this phrase during the Cold War with the Soviet Union, but it may have application today as managers and educators are evaluating the relative merits of new equipment. It is fairly easy to find product literature that describes new features and benefits, but it would be unusual to find that same literature describing any weak points or flaws.
Aerosol delivery devices can and should be put to the test, and this can be done with a minimum of effort and expense. A very simple, qualitative test can be very revealing when it comes to validating the manufacturer’s claims on aerosol output. The only materials required include a bottle of red food coloring, a filter, and a willing participant—students make excellent volunteers.
A dilute solution (approximately 10%) of red food coloring and saline is placed in the nebulizer to be evaluated. A filter is placed between the subject and the nebulizer. When everything is in place, the nebulizer is started and the subject starts breathing for a predefined period of time. When time expires, the nebulizer is stopped and the filter is removed and inspected for concentration of dye.
Figure 4 shows filters that collected aerosol from three different nebulizers. Although the same breathing pattern and the same concentration of food coloring were used, clearly there is a difference that could not be appreciated if one were to rely solely on information from product inserts.
Adding value to aerosol therapy can be accomplished in a number of ways. Some will be easier to implement than others, but the process of adding value cannot start by itself. It would be unrealistic to expect the people who decide on equipment purchases can understand that a cheaper nebulizer is not always a reasonable alternative to an expensive type.
Avoiding shortcuts with aerosol therapy is equally important as any equipment addition. Earlier in this article, Chart 1 showed that only about 12% of what gets added to a nebulizer is actually delivered to the patient’s lung. Shortcuts, like giving mask treatments to patients who can easily use a mouthpiece, only magnify the inefficiency of aerosol delivery. These types of practices should be avoided whenever possible.
Remember that the individuals most affected by these value-based decisions are the patients, but they have very little voice in the matter. The role of “advocate” should be filled by those who care enough about their craft and their patients to do what it takes to make a difference. RT
________________________________________________________
Mark Grzeskowiak, RCP, RRT, FAARC, is manager, education and quality, Respiratory Care Services, Long Beach Memorial Medical Center, Long Beach, Calif. For further information, contact [email protected].
________________________________________________________
References
1. Gardenhire D, Hess D, Meyers T, Rau J A. Guide to Aerosol Delivery Devices for Respiratory Therapists. Produced in collaboration with the American Association for Respiratory Care, 3rd edition, 2013.
2. McPeck M. Bench comparison of Circulaire II to Aeroeclipse II Aerosol Drug Delivery System (abstract). Respir Care. 2010;55(11):1564.
3. McPeck M. Financial impact spreadsheet for comparing total cost of aerosol drug delivery systems (abstract). Respir Care. 2010;55(11):1558.
4. Grzeskowiak M, McKee B, Riker J. Evaluation of the Circulaire II drug delivery system for microbiological contamination (abstract). Respir Care. 2013;58(10):1722.
5. Ari A, Telli O, Harwood R, Sheard M, Aljamhan E, Fink J. Influence of nebulizer type, position and bias flow on aerosol drug delivery in simulated pediatric and adult lung models during mechanical ventilation. Respir Care. 2010;55(7):845-851.
6. Rubin BK. Bye-bye, blow-by. Respir Care. 2001;52(8):981.
7. Bhashyam AR, Wolf MT, Marcinkowski AL, et al. Aerosol delivery through nasal cannulas: an in vitro study. J Aerosol Med Pulm Drug Deliv. 2008;21(2):181-8.
8. Ari A, Harwood RJ, Sheard MM, Fink J. Aerosol delivery through tracheostomy and endotracheal tubes. Respir Care. 2012;57:1066-1070.